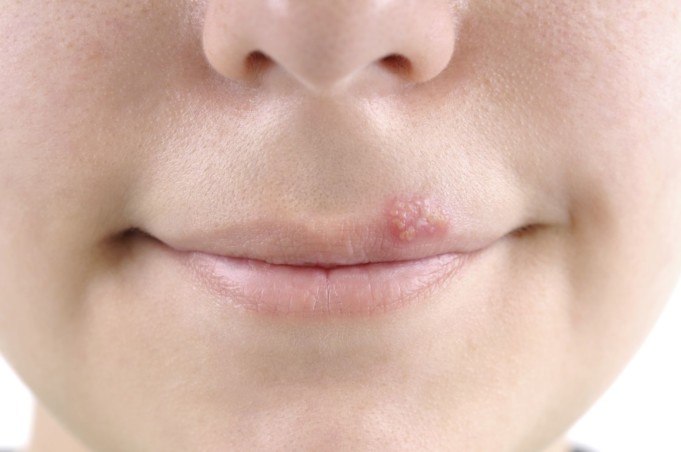
Cold sores are still medically referred to as Herpes labialis, and other familiar names include fever blisters.
It is a common viral infection caused by the herpes simplex virus. Cold sores are typically red, fluid-filled blisters that form near the lips and other facial areas.
However, in few cases, it has been observed to occur in the nose, fingers, and inside the mouth. Blisters formed by cold sores are often in groups like a patch, causing pain, itching, and a burning sensation before they break and crust over.
The most frequent cold sores are caused by a herpes simplex virus type 1 (HSV-1) infection. Other times, rarely, it is caused by an infection from another simplex virus strain called herpes simplex virus type 2 (HSV-2).
HSV can cause various infections that affect the mouth, face, skin, anal, and genital regions. It is a common chronic viral infection in humans especially, with oral herpes (HSV-1) infecting about 67% of adults worldwide, and this prevalence is higher than the prevalence of genital Herpes (HSV-2).
The herpes simplex type 1 virus resides deep in the nerve roots and may reappear later, resulting in the same symptoms in the exact location.
Cold sores alias name labia means ‘lip.’ Although the origin of Herpes labialis is the same as all herpes viral strains, it does not indicate the labia of the genitals.
When a herpes viral infection affects both the face and mouth, the broader term orofacial Herpes is used. In contrast to this term, herpetic stomatitis describes an infection of the mouth specifically.
A published article in the Bulletin of the World Health Organization in 2016 conducted a global herpes simplex type 1 and 2 infection prevalence and incidence.
In the article, Dr. Sami Gottlieb (a medical officer at WHO and author of the study) stated, “Herpes infection affects millions of individuals worldwide and can have far-reaching health effects.
WHO needs more investment and commitment to developing better treatment and prevention measures for this infection.” As of 2016, 491.5 million people lived with HSV-2; this is equivalent to 13.2% of the world’s population aged 15 to 50 years.
HSV-2 is exclusively sexually transmitted, and it causes genital and anal infections. Another estimated 3.7 billion people (estimated 66.6% of the world’s population aged 0 to 49) had HSV-1 disease in 2016.
Most HSV-1 infections were oral; but, between 122 million to 192 million persons were estimated to have genital HSV-1 infections.
This statistic depended on the assumptions used in the estimation model. The highest prevalence of these viruses appears to be in Africa and developing continents.
Cold sores are widespread among other herpes infections around the world. A survey among young adults over six continents was conducted, and it reported that about 33% of males and 25% of females had one or two times during that year had Herpes before WHO conducted the surveillance.
In the United States of America, cold sores prevalence was estimated at 20-45% among the adult population.
In France, the lifetime prevalence was reported by a study as 32% in males and 42% in females.
In Germany, the prevalence was reported in people ages 35 to 44 was 32%. While in persons aged 65 to 74, it was marked at 20%. Another study in Jordan reported a lifetime prevalence of 26%.
Causes
Cold sores are caused by two major strains of the herpes simplex virus (HSV). More frequently, it is caused by the herpes simplex type 1 virus.
But the herpes simplex type 2 virus, which is responsible for causing genital Herpes on rare occasions, may cause cold sores as complications.
Both strains can spread to the face or genitals through close contact, even through kissing and oral sex. Sharing personal care products might also spread the HSV-1 virus.
Cold sores are most painful and highly contagious when the blisters break and ooze because the virus spreads quickly through infected body fluids.
The colloquial term for this infection, “cold sores,” arises from the fact that herpes libialis is usually triggered by fever, such as during an upper respiratory tract condition (i.e., a cold).
Persons who have suffered from an episode of herpes infection have the virus lying dormant in their nerve cells in the skin, and it might emerge as another cold sore at the same spot as before.
The reemergence of cold sores may be due to:
- Viral infection of fever
- Stress
- Fatigue
- Hormonal changes (such as during menstruation)
- Exposure to sunlight or wind
- Changes related to the Immune system
- Skin breakage or injury
Stages of Cold Sores infection
There are five (5) stages to which cold sore infections have been medically classified:
- Stage1: Tingling and itching stage, about 24 hours before blisters appear.
- Stage 2: Fluid-filled blisters appearance.
- Stage 3: Blisters break, ooze, and form painful sores (highly contagious at this stage).
- Stage 4: Sores dry out and scab over, causing cracking and itching.
- Stage 5: Peeling off of scab and healing of cold sores.
Risk factors
Every age group, gender, race, and personalities are at risk of cold sore infection. Most individuals are carriers of the virus but never have they experience a symptom of the infection.
The risk of presenting a cold sore infection can increase due to the following factors:
- Weakened immune system due to medications or other conditions such as anti-rejection drugs for organ transplants
- HIV/AIDS patients
- Cancer chemotherapy
- Atopic dermatitis
- Severe burns
- Menstruation
- Stress
- Dental work
Symptoms
Some carriers of the HSV-1 may be asymptomatic. But signs and symptoms of cold sores may vary, depending on the sore stage and whether it is the first appearance or a recurrence.
If it is the first appearance of a cold sore, symptoms may not appear for up to 20 days after the first viral exposure.
A cold sore can stay as long as two weeks but, it completely heals without leaving any scars after this period. The reappearance of cold sores usually occurs at the same spot each time and tends to be less severe than the first outbreak.
At first outbreak, a person may experience:
- Painful gums
- Headaches
- Itching
- Fever
- Sore throat
- Swollen lymph nodes
- Muscle aches
Pediatric cold sores may appear inside the mouth, and the lesions are commonly mistaken for canker sores. A canker sore involves only the mucosa membrane and is not herpes simplex virus related.
Diagnosis
Doctors diagnose cold sores typically based on the symptoms presented, taking a physical examination of the blisters. Swab samples can be collected from the blisters to confirm a diagnosis, and tests can be conducted for HSV.
Differential Diagnosis
Some other conditions which may present similar symptoms to cold sore include:
- Folliculitis: This is a common skin condition caused by a bacteria characterized by a hair follicle’s inflammation and infection. When it occurs close to the lips, it may look like a cold sore outbreak.
- Oral candidiasis: This is a fungal infection of the mouth, also known as oral thrush. It is a result of candida developing on the mucous membrane of the mouth. It causes itching and burning sensations and may present swollen, slightly red spots.
- Aphthous stomatitis: This is commonly known as a canker sore. It is an ulcerative inflammatory condition of the oral cavity. But unlike cold sore, it is not contagious and does not affect the lips. However, it is still regarded as a differential diagnosis of a cold sore.
- Medication-induced stomatitis: This is very similar to a canker sore, but it is induced as a side-effect to medications. Medications include immunosuppressants, anticholinergic bronchodilators, and some antibiotics.
- Pharyngitis: Also known as sore throat, it is the inflammation of the pharynx. It may also cause itching and reddish bumps and sores close to the mouth, just like cold sore symptoms. It can either be caused by a virus or bacteria.
- Steven-Johnson syndrome: This syndrome is a rare, serious condition of the skin and mucous membrane. It is characterized by flu-like symptoms, a painful reddish rash that spreads and blisters and then begins to heal after several days, similar to rashes of a cold sore.
- Hand, foot, and mouth disease (Coxsackie coxsackievirus infection): This is a viral infection caused by a strain of coxsackievirus. The condition is known to cause blister-like rashes in the hands, feet, and mouth.
Complications
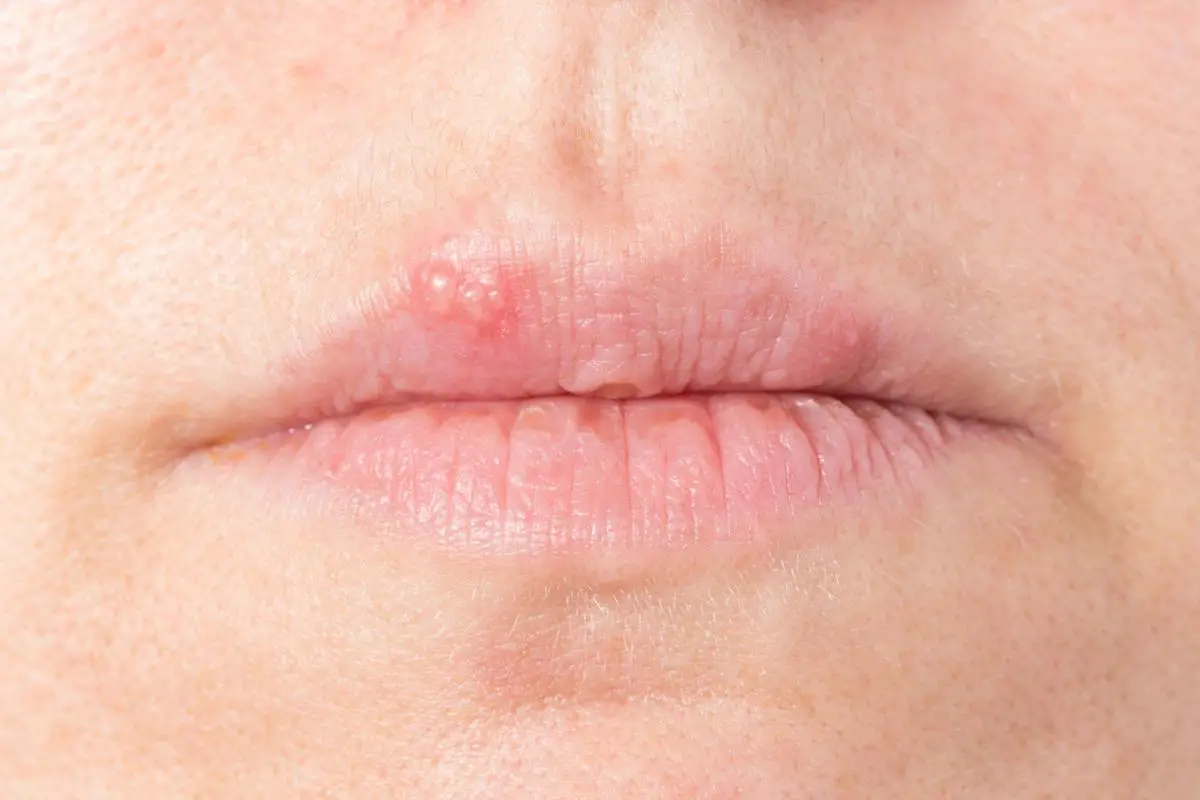
In some individuals, a herpes virus that causes cold sores can also cause problems in other areas of the body, such as:
- Fingertips: Both Herpes simplex viral strains can spread to the fingers. In this case, it results in ‘herpes whitlow.’ One common way of transmission is children who suck-on their thumbs may transfer the infection from the mouth to the fingers.
- Eyes: Herpes virus can result in eye infections when they are spread to the eyes. Repeated viral infections in the eyes can cause scarring and injury, leading to vision impairments.
- Widespread areas of the skin: People who suffer from skin conditions such as eczema are at higher risk of cold sores spreading across the body.
- High persistent fever
- Genital Herpes
- Difficulty breathing and swallowing
- Sore throats
Treatment
Cores sores are blisters fluid-filled pockets beneath the skin surface, occurring around the mouth or on the lips.
These blisters can break open, ooze, and then crust over, lasting for about ten days. Those ten days (Stages 3 and 4) can be excruciating and brutal, causing discomfort. Home remedies and natural treatments may help through this period.
The following home remedies may help but be aware that they may not work for everyone. However, antiviral OTC (over-the-counter) medications are proven to be much more effective for both the prevention and treatment of cold sores.
- Home remedies: some home techniques may be instrumental in the treatment process of cold sores symptoms. While it may not be convenient for some patient, others find these home care techniques positively effective:
– Dabbing the affected area with diluted geranium, tea tree oil, or lavender
– Appling cold, soaked tea bags to the sore every hour
– Using petroleum gel to keep the skin moist and prevent skin breakage
- Antiviral creams: These creams antiviral properties that may help reduce redness and shorten an outbreak’s duration. Most creams contain penciclovir or acyclovir, such as Soothlip and Zovirax.
- Oral antiviral medication: Such as valacyclovir (Valtrex), famciclovir (Famvir), and acyclovir (Zovirax) may be prescribed by a physician if a person has a weakened immune system or otherwise frequent outbreaks. These medications taken once or twice a day can shorten a cold sore outbreak duration and prevent reoccurrence.
- Pain relief: There is an analgesic option among OTC medications such as benzocaine or lidocaine. These medications may not shorten the duration of cold sores, but they can relieve pain and discomfort. Other relief medications include Cymex, Anbesol, Blistex, and Orajel. These ointments or gel are dabbed onto the sores with a Q-tip. If a finger is used for the application instead, the hands should be washed before and after. Some alternatives such as acetaminophen (Tylenol) or ibuprofen can be used. It is necessary to note that these products (ointment and gel) should not be shared.
Prevention
Preventive measures against cold sores are in two phases; the first is prevention to avoid HSV-1 infection. The second preventive measures are to reduce the risk of a cold sore outbreak for those already infected with the virus.
To prevent HSV-1 infection, an individual should take the following precautions around people who have cold sores:
- Do not share towels, dishes, razors, cutlery, straws, lipsticks, or lip balm with such persons.
- Always wash hands with soap and avoid touching your lips, eyes, and genitals as much as possible.
- Avoid intimate contacts such as kissing and oral sex with anyone with cold sores.
If an individual has a cold sore, they should be conscientious around babies and infants. Always wash your hands before handling one, and do not kiss a baby until the sore has completely healed.
To reduce the risk of developing a cold sore, if you have already been in contact worth HSV-1:
- Try to stay healthy as a slight fever can trigger a cold sore.
- Get enough rest as fatigue weakens the immune system and makes one more likely to get sick.
- Always wear a lip balm with SPF to protect your lips from sunburn, which can help prevent an outbreak.
Summary
Most cold sore victims learn to live with the condition and manage the outbreak by taking appropriate medications and preventive measures to avoid spreading the infection to others. Cold sores usually last for about two weeks, after which it clears up, leaving no scars or after-effects. However, immune-compromised patients, babies, and eczema persons should take more effective protective measures as cold sores can be a severe complication in such cases.
Source