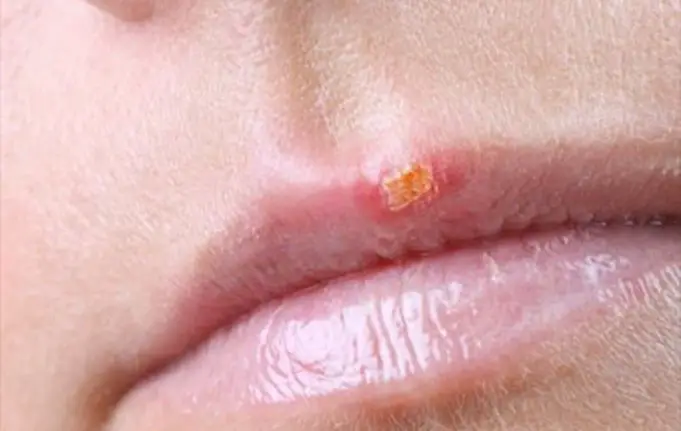
Sexually transmitted diseases (STDs) are transmitted through unprotected sexual intercourse. One of the common sexual transmitted infection is Genital herpes; it is a viral disease that any sexually active person can contact.
Most individuals living with Genital Herpes do not exhibit any symptoms and even without signs of the disease, herpes can still spread to sex partners.
This STD is caused by two types of viruses; the viruses are called herpes simplex virus type 1 (HSV-1) and herpes simplex virus type 2 (HSV-2).
Genital herpes is not a serious health threat unlike other STDs, the Centre for Disease Control and prevention (CDC) does not even recommend regular testing.
But how did herpes become so globally feared? For thousands of years, Herpes simplex has been infecting horminidae (ancient man; known to be prehistoric humans), but it was not until the year 1967 that group of scientists first distinguished between the HSV-1 and HSV-2, thereby effectively creating the concept of genital herpes.
In the following year, 1968, a team of epidemiologists at the University of Baylor declared that it had found a link between HSV-2 and cervical cancer, however, the news turned out to be false as the team misinterpreted HSV-2 for Human papillomavirus (HPV); which is an actual cause of cervical cancer.
But even at the height of the sexual revolution, with the specter of cancer attached to it, HSV-2 did not immediately invade the global imagination. In 1973, an article by a feminist magazine back quoted a doctor saying “…such is herpes simplex, a common infection, barely a disease; so why talk about it?”
In 1974, Abigail Van Buren, publicly known as Dear Abby, reassured a reader, “My medical experts inform me that Herpes-2 should not be classifies as a venereal disease and since it can be spread non-sexually, there’s no need for you to be embarrassed”.
In 1976, New York Times magazine story concluded that, herpes virus is a part of a collective ecosystem just like bacteria and pollution as it stated that the virus cohabits with humans.
But around the same decades, many other newspapers and magazines had a different sight to the issue, they called genital herpes an “epidemic” and emphasized on its incurability and laid claims that it could result in neonatal infections when passed down to infants from infected mothers during childbirth.
Modern research evaluated an overall predominance of herpes-2 rising from 13.6% to 15.7% between 1970 and 1985 but began dropping later that decade.
Ironically, one major contributor to the growth of stigmatization then among individuals with persons with herpes was testimonials from people with herpes themselves, who twisted the world’s sense of what a typical herpes diagnosis meant.
After infection, the virus may lie dormant in the body and may reactivate several times a year. Genital herpes can cause pain, itching, and sores in the genital area. Another type of herpes disease is oral herpes, which is usually caused by the simplex virus HSV-1 and can result in cold sores and fever blisters around the mouth.
However, most individuals with oral herpes were infected during childhood or young adulthood from sexual and non-sexual contact with saliva. There is a link between genital and oral herpes, as the simplex virus HSV-1 can spread from the mouth to the genitals through sex.
This is the reason why some cases of genital herpes are caused by HSV-1.
Causes of Genital Herpes
There are two different types of herpes simplex virus that causes genital herpes:
- HSV-1, this is always the cause of cold sores and oral herpes.
- HSV-2 which is the causative agent of genital herpes.
Someone can get genital herpes by having vaginal, anal or oral sexual intercourse with another individual who has the disease even if the partner does not have a visible sore or who may not know that he/she is infected.
Other ways of coming in contact with the virus and contracting genital herpes including:
- Saliva (if a partner has oral herpes infection) or genital secretions (if your partner has a genital herpes infection)
- A herpes sore
- Sweats of an infected person
- Skin in the oral area if a partner has an oral herpes infection or skin in the genital area, if a partner has a genital herpes infection.
Once the virus enters through the skin or through the mucous membranes (thin layers of tissues that lines the openings of the body for instance the nose, mouth and genitals), it travels along nerve paths.
It may become dormant as in most cases in the nerves and remain there indefinitely. From time to time, the virus may become active; by travelling along the nerve pathway to the surface of the skin, where it is shed. At this point of the cycle of the virus, it can cause an outbreak of symptoms or continue to remain undetected.
In any case, an active virus is easily passed to other persons; even wearing a condom might not be 100% safe to protect u against genital herpes as there is no condom covering the whole skin of the body.
Symptoms of Genital Herpes
Most individuals living with herpes or HSV are unaware of it because of a general absence or mild presentation of signs or symptoms of the disease.
When symptoms are present, it may begin for about 2 to 12 days after exposure to the virus.
Symptoms may include:
- Small red bumps or tiny white blisters which appear a few days to weeks after infection.
- Pain and itching may be experienced with tenderness in the genital area until the infection clears.
- Ulcerations due to rupture of blisters forms causing oozing and bleeding, it is also making it painful to urinate.
- Skin crust or scabs over old ulcerations
- Headaches, body aches and fever may be experienced.
- Swelling of the lymph glands as it fights the infection and inflammations.
- Infants who are born with genital herpes can develop severe conditions like blindness, brain damage and even death.
Risk factors for Genital Herpes
The risk of a person contracting genital herpes is on the high side if the individual:
- Woman: Women are more likely to have genital herpes than men. This is because the virus has its higher probability of the virus been sexually transmitted more easily from men to women than it is from women to men.
- Have multiple sex partners: Every additional sexual partner raises the risk of an individual being exposed to the HSVs that causes genital herpes.
- Pregnant women with genital herpes are at risk of infecting their baby with the virus during childbirth.
Prevention of Genital Herpes
The only major to avoid contracting STDs is abstinence from illicit sexual activities. If one is sexually active, the following measures can be observed to at lower the risk of getting genital herpes:
- Keeping a long-term mutually monogamous relationship with a partner who is uninfected with an STD (partners who have tested negative to STDs including Genital herpes)
- Using latex condoms, the right way during every sex time, though this does not totally herpes however, it greatly reduces the risk of infection.
If a partner already has genital herpes, the uninfected partner can do the following to prevent been infected with genital herpes and still keep a healthy relationship:
- Ensure the infected partner takes appropriate medication against the STD. the infected partner should openly discuss with a doctor.
- Vaginal, anal and oral sexual activities should be avoided when the partner has the symptoms.
During Pregnancy, a lady who is infected with genital herpes should ensure to inform the doctor early and it is very important she pays visits to prenatal care. Inform the doctor about symptoms experienced or have been diagnosed with genital herpes.
Also, information about her partner’s statue will be highly useful. There is some research that suggests that genital herpes infection may lead to miscarriage or could induce premature delivery.
Infection from herpes can easily be passed from a mother to her child before birth or during delivery, and this potentially leads to deadly infection in the child (known as neonatal herpes).
Because of this reason, it is very important that a woman avoid herpes during pregnancy. In cases of infection during pregnancy, the woman is placed on herpes medication towards the end of the third trimester.
This medication helps reduce the symptoms of herpes at the time of delivery, however, if herpes symptoms are still noticed at delivery, a C-section is usually performed.
Diagnosis of Genital Herpes
Typically, genital herpes is diagnosed by a physical examination of the herpes sore (If any). Although to save time, physical examinations are not always necessary as the clinician can confirm diagnosis through laboratory blood tests.
This blood test can be used to confirm the presence of the HSV in the bloodstream even without patients exhibiting symptoms.
Treatment of Genital Herpes
Treatment approach to genital herpes usually reduces the outbreaks but it cannot cure herpes simplex viruses. It can only suppress the activity of the virus.
Medications like antiviral drugs can greatly enhance the healing time of herpes sores and reduce pain. Medications can also be taken at the first sign of an outbreak to help fight symptoms. Individuals who experience outbreaks may also be prescribed medications to minimize the chances of future occurrence, as it is likely to frequently occur in persons with suppressed immune systems.
For Home care and management of herpes, the use of mild cleansers and antiseptic when bathing or showing in warm water is always prescribed.
Infected sites of sores should be kept clean and dry, as sores can be transferred to other parts of the body if the fluid from the sore touches an unaffected site. If sores are touched, hands should be washed immediately to avoid spreading. Pregnant women with herpes should always consult a doctor.
Some other activities can be done at home to relieve the discomfort and severity of symptoms during an outbreak, these home treatments include:
- Taking of painkillers such as acetaminophen, ibuprofen or aspirin.
- Letting air circulate around sore sites by wearing loose-fitting clothing.
- Putting ice parks on the affected area. Ice should be wrapped in a towel or piece of clean cloth.
- Get plenty of rest.
- Avoid oral sex when either partner has oral or genital sores.
- Do not wet your contact lenses with saliva.
- Do not kiss when you or your partner has cold sores.
- Do not have genital or anal contact when any sores are present.
Conclusion: Genital Herpes comeback and HIV
In a comeback case of genital herpes case which is not so rare especially in low immune system individuals following an expected outbreak of three to four times yearly, regular antiviral should be taken as with time, this will help the body system build up more immunity to the virus and the comebacks may become less frequent, even coming to an end in some persons.
These comes may be linked to some other causes. In recorded cases, conditions like fatigue, illness, sexual intercourse, menstruation, stress, surgery, and trauma.
Finally, most persons and patients alike are always concerned if genital herpes has any link with HIV (Human Immune deficiency Virus).
Well, Genital herpes infection actually causes sores and breaks in the skin or lining of the mouth, vagina, and rectum which are subsequent openings for HIV to enter the body.
Even without visible sores, been infected with genital herpes increases the number of CD4 cells- the cells that HIV targets for entry into the body, found in the lining of the genitals.
When a person is the carrier of HIV and still infected with genital herpes, the chances of spreading both STDs are very high during sexual contact via the mouth, vagina, or rectum?
Sources;
- Genital Herpes; Http://www.nhs.uk/conditions/genital-herpes/
- Symptoms of herpes; http://www.plannedparenthood.org/learn/stds-hiv-safer-sex/herpes/what-are-the-symptoms-of-herpes