As the heartbeats, it pumps blood into a series of blood vessels, called the circulatory system. The vessels are hollow, flexible tubes carrying blood to any part of the body. Oxygen-rich blood is transported away from the heart by arteries, while oxygen-poor blood is returned to the heart by veins.
The veins are flexible, hollow tubes with flaps inside called valves. The valves open when your muscles contract and permit blood to flow through the veins. It also closes as the muscles relax, keeping blood circulating into the veins in one direction. The veins get bigger as they get closer to the heart.
The superior vena cava is a large vein that carries blood into the heart from the head and arms, while the inferior vena cava carries blood into the heart from the abdomen and legs.
If, as a result of vein disease, also known as venous disease, the valves inside your veins become weakened, the valves can not close properly. This causes blood to leak backward or flow in both directions.
What are vein diseases?
Vein disease includes the following:
Blood clots
It can be found in the legs, arms, veins of the inner organs (kidney, spleen, intestines, liver, pelvic organs), in the brain (thrombosis of the cerebral vein), in the kidneys (thrombosis of the renal vein), or the lungs (pulmonary embolism).
Deep vein thrombosis
Deep vein thrombosis (DVT) is a blood clot formed in a deep vein (including upper extremity (arms) and lower extremity (legs). Although deep vein thrombosis is not life-threatening, the blood clot has the ability to break free and pass through the bloodstream, where it can become trapped in the blood vessels of the lung (known as a pulmonary embolism). This can be a life-threatening problem.
Superficial venous thrombosis or phlebitis
Superficial venous thrombosis is a blood clot, which occurs in a vein close to the skin surface. If they pass from the simple system into the deep venous system first, these forms of blood clots generally do not migrate to the lungs. Nevertheless, they usually cause pain.
Chronic venous insufficiency
Chronic venous insufficiency, known as venous stasis ulcer, is distinguished by blood pooling, a chronic swelling of the leg, intense pressure, increased skin pigmentation or discolouration, and leg ulcers.
Ulcers
Ulcers induce static blood flow or venous stasis ulcers. Ulcers are bruises or open sores which do not heal completely as they tend to keep coming back. Ulcers of venous stasis are situated below the knee and are mainly found just above the foot, on the inner part of the body.
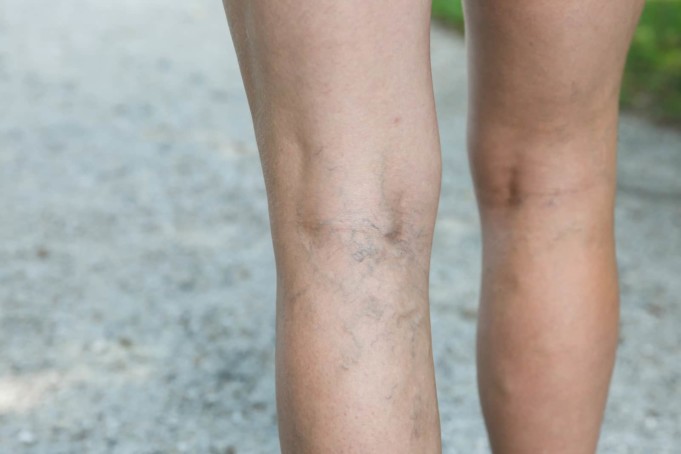
Varicose and spider veins
Varicose and spider veins are abnormal, dilated blood vessels triggered by a weakening in the blood vessel wall.
Symptoms
The varicose vein may not induce any distress. However, there are signs that you show one have varicose vein disease:
- Veins that are dark purple or blue
- Veins that looks twisted and are bulging are very much like cables on your legs
If there are painful symptoms, they may include:
- A tense or achy sensation in your legs
- Burning, throbbing, muscle pain, and swelling in your lower legs
- Worsened discomfort after a long period of sitting or standing
- Itching along with one of your veins or more
- Decolourationof the skin around a varicose vein
Varicose veins are identical to spider veins, but they are narrower. Spider veins can be seen closer to the surface of the skin and are mostly red or blue.
Spider veins appear on the legs but can also be located on the face. They differ in size and often look like the web of a spider.
Causes
Varicose veins may result from weak or impaired valves. The arteries bring blood to the rest of the tissues from the heart, and the veins carry blood to the heart from the rest of the body so that the blood can be recirculated.
The veins in your legs work against gravity in order to return blood to your heart. Muscle contractions in your legs serve as pumps, and flexible vein walls enable blood to return to your heart.
As blood flows into your heart, tiny valves open in your veins, then close to prevent backflow of blood. Blood may flow backward, allowing the veins to stretch or twist if these valves are weak or impaired.
Risk factors
These factors below increase your chance of developing varicose veins:
- Age: The chance of varicose veins rises with age. Ageing in your veins induces wear and tear on the valves that help control the flow of blood. Ultimately, the damage causes the valves to permit blood to flow back into the veins where it gathers rather than just flowing to the heart.
- Sex: Women have greater chance of developing the disorder. As female hormones appear to relax vein walls, hormonal changes during pregnancy, pre-menstruation, or menopause can be factors. Your risk of varicose veins can be increased by hormone therapies, like birth control pills.
- Pregnancy: The amount of blood in the body rises during pregnancy. This helps the developing fetus, but it can also cause an unfortunate side effect: swollen veins in your legs. Hormonal shifts can also play a function during pregnancy.
- Family history: If there are varicose veins in other family members, there is a greater risk that you will get it.
- Obesity: Being obese places extra strain on your veins.
- Standing or sitting for extended periods: When you’re in the same place for long stretches, the blood does not flow well.
Prevention
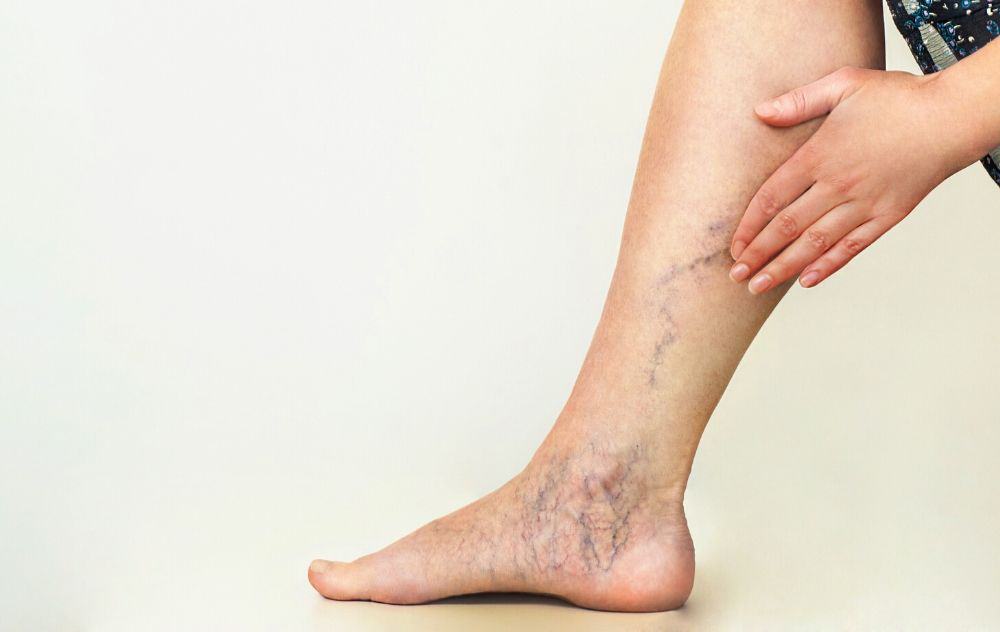
There is no way to avoid varicose veins entirely. However, by strengthening your circulation and muscle tone, it can reduce the risk of having varicose veins or getting extra ones.
The same steps you should take to treat varicose vein pain at home can help to avoid varicose veins, including:
- Exercising
- Observing your weight
- Eating a low-salt, high-fibre diet
- The avoidance of high heels and tight trousers
- Elevating your legs
- Regularly adjusting your sitting or standing position
When to see a doctor?
Self-care, such as exercise, raising your legs, or wearing compression stockings, may help you relieve the pains of varicose veins and keep them from getting worse. But see your doctor if you’re worried about how your veins look and feel or if self-care strategies have not prevented your condition from getting worse.
Reference;
- Varicose vein – mayoclinic
- Venous vein – Clevelandclinic