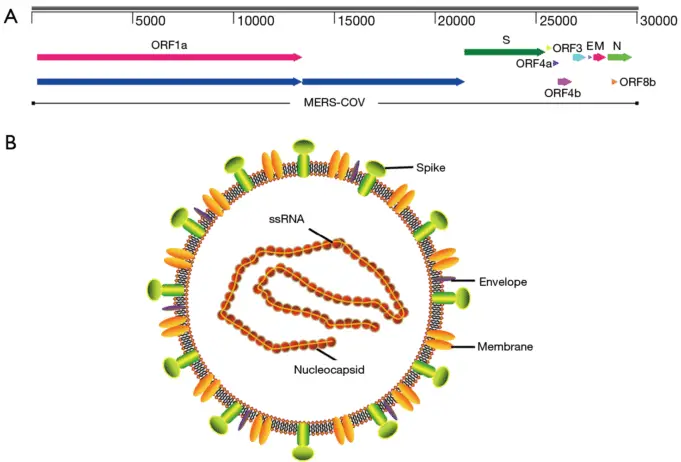
Middle East Respiratory Syndrome (MERS) is gaining attention yet again because of the recent case of the coronavirus outbreak in China. MERS is an illness that is caused by a coronavirus known as the Middle East Respiratory Syndrome Coronavirus (MERS-CoV).
Most people who caught the MERS virus developed very severe respiratory sickness with cough, symptoms of fever as well as shortness of breath. It is estimated that 3 or 4 out of each 10 patients that caught the MERS coronavirus have died.
All cases of the MERS virus are linked to the Arabian Peninsula
The first time Health officials reported the MERS disease was in September 2012 in Saudi Arabia. Through retrospective investigations, health officials later discovered that the first known cases of MERS was recorded in Jordan in April of 2012.
From the time of the first outbreak till now, all cases of MERS have been transmitted through residence in or travel to countries in and around the Arabian Peninsula.
The biggest recorded outbreak of MERS outside of the Arabian Peninsula was recorded in the Republic of Korea in the year 2015. The outbreak in Korea was connected with a traveler coming back from the Arabian Peninsula.
People who have MERS can spread it to other people in several ways.
MERS-CoV has been recorded to spread from an ill person to others through direct contacts, such as touching, caring for, or living with an infected person.
Anyone can be affected by the MERS coronavirus. MERS is not an age-specific illness from people who are younger than 1 year of age to those who are 99 years old.
The CDC made sure to monitor the global MERS situation closely. They worked closely with partners to understand the risks of the virus better, including its origin, how it spreads, and the best possible ways to prevent infections.
Symptoms
Most people who were confirmed to have MERS-CoV infection have suffered severe respiratory illness with symptoms such as:
Some people who were diagnosed with MERS also had nausea/vomiting and diarrhea. For many individuals who had MERS, some severe complications such as kidney failure and pneumonia followed.
As mentioned about, 3 or 4 out of each 10 people who were reported to have MERS have died. However, most of the people who died from the MERS virus were discovered to have a pre-existing medical condition that causes their immune system to become weakened or an underlying health challenge that had not yet been found.
Medical conditions can sometimes weaken a person’s immune systems and cause them to be more likely to fall sick or suffer from severe illness.
Some Pre-existing conditions among people who were diagnosed with MERS included
- Diabetes
- Cancer
- Chronic lung disease
- Chronic kidney disease
- Chronic heart disease
Some of the people who got infected had mild symptoms like cold-like symptoms or no noticeable symptoms at all.
The symptoms of MERS start to show up about 5 or 6 days after the first exposure to the virus but are known to range between 2 to 14 days.
MERS-CoV, just like other coronaviruses, spreads from respiratory secretions of an infected person, such as through sneezing, coughing. However, health professionals do not entirely understand the exact ways that it spreads.
MERS-CoV has spread from people who are ill to others like caregivers and through close contact. People who were infected were found to spread the virus to other people in hospitals and other healthcare settings.
Researchers who studied MERS did not see any spread of MERS-CoV in the community.
Prevention
There is still no vaccine to protect against MERS coronavirus. But scientists are currently working to develop one.
Nevertheless, the following preventive measures can be helpful during an outbreak:
Wash your hands thoroughly as often as you can with soap and water for no less than 20 seconds, and make sure to help children do the same. In the absence of soap and water, use an alcohol-based hand sanitizer.
Cover your mouth and nose with a handkerchief and tissue when you sneeze or cough, then dispose of the tissue properly in the trash.
Avoid using your unwashed hands to touch your eyes, nose, or mouth.
Avoid all forms of personal contact with an infected person. Contacts such as sharing cups, kissing, or using the same eating utensils with people who are sick.
Clean and disinfect all objects and surfaces that are frequently touched, such as doorknobs.
If you are living with or caring for a person confirmed to have MERS, or have been evaluated for, a MERS-CoV infection, take precautionary measures.
Treatment
There is no particular antiviral treatment that has been recommended for MERS-CoV infection. People who have MERS often get medical care to alleviate symptoms.
For severe cases of MERS, current treatment includes medical supervision to support the function of vital organ