Have you ever gone to the toilet, and after using it, you notice blood in your stool? Then you probably may be suffering from rectal bleeding. Rectal bleeding occurs when blood is found passing through your anus.
Sometimes, doctors refer to rectal bleeding as the bleeding that comes from your anus, lower part of your colon, otherwise known as your sigmoid colon or from your rectum.
Your large intestine is made of about five sections, namely your ascending colon, your transverse colon, your descending colon, your sigmoid colon as well as your rectum.
As such, it can be said that your rectum is the last part of your large intestine. If anything irritates your rectum to bleed or any region of the lower part of the large intestine to bleed, it will cause rectal bleeding to occur.
Rectal bleeding sometimes may be seen as blood in your stool, blood on your tissue paper, or blood on the toilet seat. One may notice that the blood seen is not bright red.
Sometimes, it may be purple, maroon, or black. The color of the blood seen depends on the location of the bleeding. Generally, doctors have speculated that the closer the bleeding is to the anus, the brighter the color is.
This means that if the bleeding occurs far up the large intestine, the color may become purple or maroon. However, bleeding from the rectum, the sigmoid colon and the anus tends to be red, and this is because these sites are closer to the anus.
The medical term for rectal bleeding is hematochezia. The severity of the bleeding mostly depends on quite a lot of factors.
Causes of rectal bleeding
Rectal bleeding is often caused by a number of factors. These factors include the following:
- Hemorrhoids
- Anal fissure
- Anal fistula or abscess
- Diverticulitis
- Inflammatory bowel disease, often known as IBD.
- Ulcers
- Large polyps.
Hemorrhoids
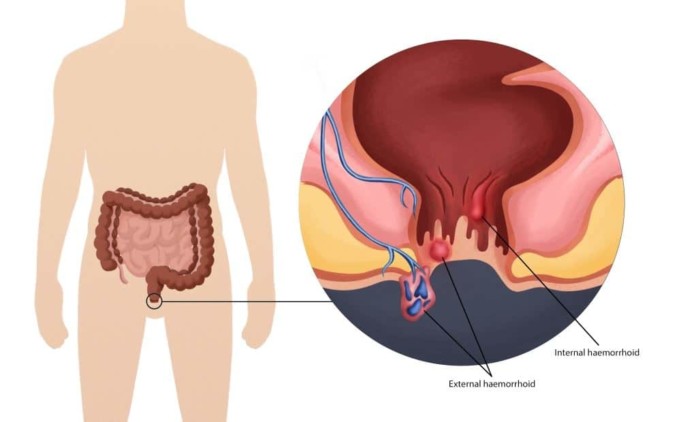
Hemorrhoids occur as a result of swollen veins within the rectum or the anus. Hemorrhoids are often a common cause of rectal bleeding, and depending on their location, they can be divided into two, namely; external hemorrhoids (hemorrhoids found in the anus) and internal hemorrhoids (hemorrhoids found in the rectum).
A common name for hemorrhoids is Pile, and it is usually developed as a result of constipation, which always occurs over a long period (chronic constipation), severe strains from work especially jobs that have to do with heavy lifting, straining while stooling, anal sex as well as obesity.
To treat hemorrhoids, mostly, it is preferable first to address the underlying cause. Doctors often try to treat the cause of the straining and constipation, and as a result, hemorrhoids are taken care of. A change in work habits, too, has been seen to treat hemorrhoids effectively.
If, after treating the underlying cause, the Pile is still present, then surgery is needed in order to arrest the rectal bleeding. The surgical process may include any of the following methods.
a. Rubber band ligation:
This process is done by the application of a rubber band, which is placed at the base of hemorrhoids. What this does is that it helps to cut the blood supply and circulation to hemorrhoids.
Once this is done, hemorrhoids will shrink away as a result of the lack of blood supply, and as such rectal bleeding stops.
b. Sclerotherapy:
This process is mostly done using the injection of a particular chemical just around the large swollen vein. This chemical will cause the shrinkage of the vein effectively treating hemorrhoids, and as such, the rectal bleeding is arrested.
c. The use of Lasers and Infrared:
This is often done when the hemorrhoid is a small one. Hence, a precise laser beam or infrared is used to burn the hemorrhoid is burnt away.
d. HET procedure:
This is a procedure that is used to treat small hemorrhoids. Unlike the precise laser beam, in this procedure, a bipolar device is used to burn the small hemorrhoids present in the vein.
This procedure is considered to a minimally invasive procedure, and it can be done in an endoscopy suite or under vision in an office.
e. Hemorrhoidal Arterial Ligation:
As the name implies, this process is done using a Doppler probe to locate the blood vessels that are responsible for supplying where the hemorrhoids are, and then those blood vessels are tied.
This process effectively causes hemorrhoids to shrink, treating the rectal bleeding.
f. Hemorrhoidectomy:
This is a process that is done surgically. This process represents the surgical removal of the hemorrhoids.
Anal Fissure
Anal Fissure occurs when there is a tear or splits along the internal lining of the uterus. This tear causes a painful burn just after passing out stool as well as bleeding.
Anal Fissure is mostly caused by the strained passing of a hard stool, which in turn causes a spasm of the anal sphincter muscle.
Anal Fissure is often a protective measure that the body uses. What occurs is that if the person already has an existing anal fissure and he or she passes out a hard stool, the stool will end up expanding the already existing tear and as such, bleeding starts.
Sometimes, doctors have mistaken anal fissures as hemorrhoids, but they both are entirely different. Fissures are a result of a tear in the lining of the anal wall, while hemorrhoids are as a result of a swollen vein.
Fissures often don’t require treatments as they tend to get resolved on their own.
However, if a fissure doesn’t resolve itself, then the application of medication or ointments as the treatment directly on the fissure can resolve the tear and pain. Some fissures which are often regarded as chronic ones won’t be able to heal without surgery.
Perianal abscesses
Typically, there are certain small glands that open into the anus. Doctors speculate that the reason for the presence of these glands is to help in the passing out of the stool.
Once any of these glands become blocked, it can cause the formation of pus, causing an infection and, as such, leading to an abscess.
The draining of the abscess can be carried out in a doctor’s office using local anesthesia.
Anal Fistula
A fistula can be defined as the joining of two structures or two spaces. An anal fistula occurs when there is a bridge of skin joining the anus or the rectum to the skin that is found around the anal region.
Fistula always first present as a result of an infection in the anal gland, which is a gland that is usually found in the anus. An anal fistula is mostly caused by an infection found in the perianal area.
Asides an infection, inflammatory bowel disease(IBD), constant radiation as well as tuberculosis can cause the formation of an anal fissure. Unlike perianal abscesses, anal fistula would require a surgeon in order for him to treat the condition.
Anal diverticulitis
Diverticulitis, otherwise known as diverticulosis, is said to occur when a small pouch or pocket is developed from weakened parts of the linings of the intestinal wall.
Once this pouch is formed, it tends to protrude through the walls of the bowels, mostly through the sigmoid colon.
Diverticulitis is a common occurrence among the elderly in western societies, and to detect it, a doctor will have to make use of an endoscope into the sigmoid colon (sigmoidoscopy) or the colon (colonoscopy).
Although diverticulitis is a benign non-cancerous growth, however, it causes rectal bleeding, which is one of its most prominent symptoms. It can also lead to bowel disorders, abdominal pain, fever, and a sudden change in bowel routines.
Inflammatory bowel disease
This disease occurs as a result of the swelling or inflammation of the bowels (which includes the small and large intestines). Generally, there as two kinds of inflammatory bowel disease, and both can lead to rectal bleeding.
They include;
- Crohn’s disease: Crohn’s disease is characterized by patterns of inflammation occurring everywhere along the entire length of the digestive tract.
- Colitis: Colitis generally has to do with the inflammation of the large intestine, otherwise known as the colon.
8. Ulcers
Ulcers are another common cause of rectal bleeding. Ulcers are known as injuries or sores that are present within the stomach lining or the first part of the small intestine, commonly referred to as the duodenum.
Ulcers are caused by the imbalance between the gastric juices present in the stomach and the digestive fluids present in the duodenum. Abdominal pains are the most common symptom a patient who has ulcers observes.
When ulcers become severe without treatment, it can lead to rectal bleeding.
9. Polyps
One primary reason why it is risky to ignore rectal bleeding is due to the fact that it can be a vital sign of cancer of the colon and/or the rectum, which is often known as colorectal cancer.
Colorectal cancer is one of the most common forms of cancers around, and it is easy to be treated, provided someone can go for early diagnosis and detection.
Cancer of the colon or the rectum is often caused by the abnormal growth of cells and tissues within the large intestines, which in turn will lead to the formation of polyps.
A polyp is a mushroom-like substance that is attached to the linings of the large intestine. Once the polyps begin to grow bigger, they will start to cause rectal bleeding.
Although the majority of polyps formed are considered to be non-cancerous, there are certain types that will end up causing cancer if left untreated for an extended period.
Doctors always advise that it is better to remove polyps once they are developed as this process can prevent the development of cancers.
The early stages of colorectal cancer can be a bit difficult to detect, and this is because they hardly produce any signs and symptoms.
However, for individuals who are considered to be at risk, they are encouraged to always go for routine screening, as this will help detect any formation that may have occurred.
Symptoms of rectal bleeding
The symptom of rectal bleeding is the presence of blood anytime you use the toilet or anytime you stool. You may likely experience abdominal pain, but more often than not, rectal bleeding occurs as a painless process.
Treatments of rectal bleeding
Generally, rectal bleeding takes care of itself. However, treatment will depend on the cause of the bleeding. If the cause of the rectal bleeding is hemorrhoids, taking of regular warm baths can help relieve the symptoms as well as it may help resolve it.
Likewise, the application of over-the-counter drugs as well as prescription creams has been seen to be very useful when applied to the place or site of irritation.
If the hemorrhoid is a large one, then your doctor might have no option but to perform invasive surgery. Your doctor may have to decide if he should use rubber band litigation, laser treatments, or surgical removal.
He or she will make this decision based on the severity of the pain caused by the hemorrhoids or the amount of bleeding which may have occurred.
For anal fissures, they do have the tendency to resolve themselves on their own. However, if they aren’t resolving themselves on their own, then your doctor may prescribe the use of stool softeners, which will help soften your stool anytime you feel the need to go to the toilet.
Stool softeners also will help decrease constipation and increase the frequency of the usage of the restroom. They also help in the treatment of anal fissures. However, if there is already an existing infection, your doctor will prescribe antibiotics to help fight the infections.
If you have colon cancer as the cause of the rectal bleeding, your doctor may need to perform a more invasive procedure, radical and long-term treatments.
These treatments will include surgery, radiation as well as chemotherapy in order to remove cancer and also reduce the risk of it reoccurring or relapsing again.
There are some home treatments that can help in preventing constipation and ultimately prevent rectal bleeding fro occurring.
These treatments include;
- Eating foods that are very rich in fiber
- Exercise regularly in order to prevent constipation.
- Ensure that your rectal region is kept clean. Always ensure that you leave this area neat, especially after using their toilet.
- Never forget to stay properly hydrated.