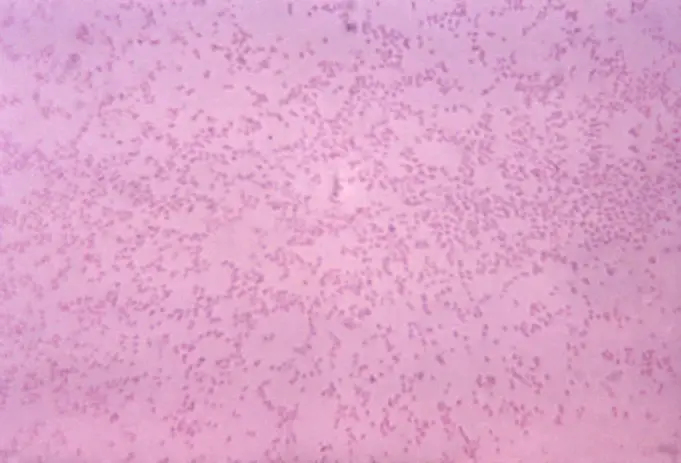
Pasteurellosis is an infection caused by bacteria of the genus Pasteurella. It is a zoonotic disease which commonly attacks cattle, dogs, cats, chickens, and some other animals. Pasteurella multocida is the most common cause of Pasteurellosis.
P. multocida is a small Gram-negative bacillus found living in the mouth and respiratory tracts of animals such as dogs, pigs, and cattle. It is a commensal and pathogen in different animal species.
Pasteurellosis may sometimes be referred to as Shipping Fever. This is a type of Pasteurellosis that attacks cattle under stress during shipping. This fever is followed by respiratory difficulty and in turn leads to pneumonia. This type of Pasteurellosis is caused by Pasteurella haemolytica.
Pasteurellosis can also lead to pneumonia in sheep and septicemia in other animals. In humans, Pasteurellosis may occur as a result of bites or scratches from cats or dogs leading to soft tissue infection and some medical complications.
Symptoms in Humans
Infected humans may show and experience symptoms after 3hours of bite or scratch. These symptoms may include;
- Swelling of wounds
- Redness of wound
- Purulent discharge
- Severe pains
- Moderate or high fever
- Vomiting, headache and diarrhea may occur
Causes of Pasteurellosis
In Human:
Pasteurellosis in human is caused by exposure to domestic animals or pets like dogs and cats. A bite or scratch from these animals can leave a wound and result to wound infection. This wound infection develop to a soft tissue infection and abscesses or osteomyelitis
Pasteurellosis can also cause respiratory infection and meningitis in humans having underlying pulmonary diseases.
In Animals:
The organism Pasteurella multocida is found living in the upper respiratory tract (nasopharynx and proximal gastrointestinal tract) of healthy animals. Hence, it is a part of the normal flora of these animals. These animals include domestic animals; dogs, cats and livestock including chicken, cattle and swine. Pasteurella multocida may cause respiratory disease in cattle.
Transmission
In Humans:
Pasteurella Spp. especially P. multocida is transmitted to humans directly by animals (dogs and cats) through scratch or bites. These animals are carriers and may not exhibit any symptoms of illness.
In absence of direct contact with the infectious secretions from these animals, infection may also occur from animals licking humans. Contact with infectious secretion or excretions can cause Pasteurellosis.
In other words, when a human uses an item contaminated by these infectious secretions or excretion the organism is being spread. This is an indirect transmission of the infection.
Three hours on exposure to bites or scratch from dogs or cats, pains, swelling and redness around the wound may occur within 12 to 24hours causing a discharge of pus.
Sepsis may occur with mild fever. Complications may include, formation of abscess, edema and osteomyelitis. This is referred to as a local infection.
Respiration infection:
P. multocida may cause severe pneumonia, trauma, infection and immune compromise in humans most especially in patients with chronic underlying respiratory disease.
In Animals:
In animals, transmission of Pasteurella multocida may occur through direct contact with infectious excretions or secretions and indirectly with fomites. P. multocida being a commensal in animals, its infection in animals can be induced by stress.
Such stress include transportation stress, heat stress, overcrowding, introduction of new animals or concurrent disease.
Diagnosis of Pasteurellosis
Pasteurella multocida is diagnosed by isolating the organism in blood, pus or cerebrospinal fluid which are normally sterile.
Treatment
The wound from animal bites or scratch should be properly cleaned and treated. It is advised to seek medical attention even as antibiotics can or may prove effective in the treatment of Pasteurella infection.
Usually, a high dose of penicillin is used to treat Pasteurellosis if severe.
Drugs like Co-amoxiclav may be effective against Pasteurella in setting and treatment of wound infection. Tetracycline or Chloramphenicol can be used to treat Pasteurellosis in patients that are beta-lactam intolerant. Susceptibility testing of isolates can be employed.