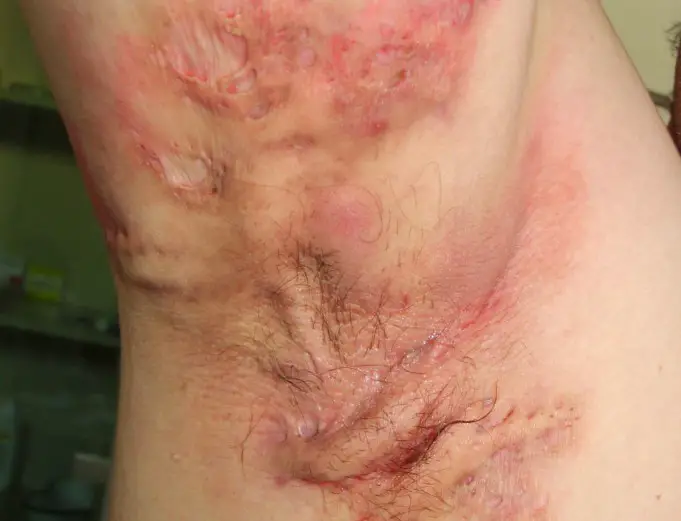
Hidradenitis suppurativa (hi-drad-uh-NIE-tis sup-yoo-ruh-TIE-vuh) iS is a skin disorder that causes the skin to form small, painful lumps. The lumps can break open, or underneath the skin can form tunnels.
The disease mostly affects places such as the armpits, groin, buttocks and breasts where the skin rubs together.
After puberty, Hidradenitis suppurativa tends to start. It can continue and worsen over time for several years, with severe effects on your everyday life and emotional well-being. Medications and surgery can help to avoid complications and manage symptoms.
Symptoms
Hidradenitis suppurativa can affect one spot or multiple parts of the body. Signs and symptoms of the condition include:
- Blackheads. A typical characteristic is small pitted areas of skin that contain blackheads, sometimes occurring in pairs or a “double-barreled” pattern.
- Painful lumps that are pea-sized. Typically, the disease begins with a single, painful lump under the skin that lasts for weeks or months. More bumps will form later. They typically occur in places where many oil and sweat glands have hair follicles, such as the groin, the armpits, and the anal area. They also occur when skin, such as the inner thighs, breast and buttocks, rubs together.
- Tunnels. Tracts connecting the lumps can form under the skin over time. These wounds, if at all, heal very slowly and may leak pus, which may have a smell.
Any individuals with this disorder experience minor symptoms only. Symptoms can be exacerbated by extra weight, stress, hormonal changes, heat or humidity. In women, the severity of the disease after menopause may decrease.
When to see a doctor
Early detection of hidradenitis suppurativa is critical to getting effective treatment. See your doctor if your condition:
- That’s painful
- If In a few weeks, doesn’t improve
- Returns in the weeks following treatment
- Appears in many areas
- Also flares
If a diagnosis of hidradenitis suppurativa has already been made, bear in mind that the warning signs of a flare of the disease are mostly close to those that originally occurred. Pay heed to any emerging signs or symptoms as well.
This can mean either a flare or a treatment complication. You will need to see a skin disease doctor (dermatologist) for long-term treatment or a surgeon.
Causes
There is no known specific cause of hidradenitis suppurativa. When hair follicles in the skin become blocked, hidradenitis suppurativa can occur.
Experts say it may be due to hormones, genes that are inherited and problems with the immune system. A function may also be played by smoking, excess weight and metabolic syndrome.
Hidradenitis suppurativa is not caused by an infection or being unclean, and it can’t be spread to other people.
Risk factors
Factors that increase your chance of developing hidradenitis suppurativa include:
- Age. In women between the ages of 18 and 29, Hidradenitis suppurativa most frequently occurs. People who develop the disorder may be at increased risk of developing more common illnesses at an early age.
- Sex. Hidradenitis suppurativa is more likely to occur in women than in men. Past of families. It is possible to inherit a propensity to develop Hidradenitis suppurativa.
- With obesity. A link between being overweight and hidradenitis suppurativa has been demonstrated in several studies.
- Tobacco. Hidradenitis suppurativa has been associated with smoking tobacco.
Hidradenitis suppurativa, which is chronic and serious, frequently causes complications, including:
- Infection. The area affected is prone to infection.
- Scars and altered skin. The wounds can heal but leave scars or pitted skin rope-like.
- Limited movement. Sores and scar tissue, especially when the disease affects the armpits or thighs, can cause restricted or painful movement.
- Drainage of obstructed lymph. Many lymph nodes also comprise the most popular locations for hidradenitis suppurativa. Scar tissue can interfere with the drainage system of the lymph, which can cause swelling of the arms, legs, or genitals.
- Social loneliness. The place, drainage and odour of the sores can result in public humiliation and reluctance to go out, contributing to depression or sadness.
Diagnosis of Hidradenitis suppurativa
Your doctor will observe the signs and symptoms, monitor your skin, and take your medical history with you.
To diagnose hidradenitis suppurativa, no laboratory test is available. But if there is pus or drainage, your doctor might send a sample of the fluid for testing to a laboratory. Other factors, such as an illness, may help rule out this.
Treatments
Drugs therapy, surgery, or both can help to manage symptoms and avoid complications. No single option has been proven to be absolutely effective, and the best combination continues to be determined by testing. Discuss the costs and advantages of the different treatment options with your doctor and create an approach tailored to your situation.
With the dermatologist or a multidisciplinary health care team, plan to have frequent follow-up appointments that will include the comprehensive care often needed by people with hidradenitis suppurativa.
Drugs
One or more of the following types of drugs may be recommended by your doctor:
- Antibiotics. With topical creams that combat infections, such as clindamycin and gentamicin, mild symptoms could be controlled.
- Systemic drugs. Some drugs are taken orally, such as clindamycin, rifampin, and doxycycline can help with more widespread diseases. Adalimumab injection may be used for mild to serious illnesses, but it may take around two weeks for any benefits to be seen. And small trials have shown the efficacy of the injectables infliximab and anakinra.
- Painkillers. Your doctor can recommend a stronger form if over-the-counter pain relievers don’t help.
Surgery
Surgical options include:
- Exposing the tunnels. This process, known as unroofing, involves scraping tissue to uncover the tunnels under the skin. It is used for people with hidradenitis suppurativa, which is mild to extreme. Usually, this solution does not have to be replicated.
- Punch Debridement. Restricted unroofing is often referred to as this technique which can be used to extract a single inflamed nodule.
- Tissue-sparing excision with electrosurgery. For individuals with serious hidradenitis suppurativa, this may be a choice. It combines electrosurgical peeling with skin-tissue-sparing removal (excision) of damaged tissue.
- Lasers Therapy. To make lesions go away, carbon dioxide lasers can be used.
- Surgical Removal. For individuals with recurrent or serious symptoms, surgical treatment may be an option. It includes all of the skin affected is removed. To close the wound, a skin graft may be required. Sores in other areas can still occur even after you have surgery. Surgical removal of the scrotum is almost always required in men whose condition includes the area between the anus and scrotum.
- Drainage and incision. An important alternative for the treatment of hidradenitis suppurativa is no longer considered to be surgical drainage. In order to provide short-term pain relief, the technique can be considered, but sores appear to flare again.
In order to improve treatment for hidradenitis suppurativa, more studies of surgical options are required. In particular, to determine the timing of surgery and form of surgical procedure, good-quality clinical trials are needed.
Topical antiseptics, experimental biological therapies and further research of adalimumab are other interventions being tested.
Lifestyle and remedies at home
Mild hidradenitis suppurativa can only be handled with measures of self-care. Yet self-care is also an important addition to any medical treatment you may receive. The following guidelines can help ease pain, accelerate healing or avoid outbreaks:
Follow a regimen of everyday skincare. With a non-soap cleanser like Cetaphil, gently wash your body. Using an antiseptic wash such as chlorhexidine will help to indicate 4 per cent. Try it once a week first, then raise intake up to once a day if your skin tolerates it well.
Stop using washcloths, loofahs or other products on impacted areas while washing. They can irritate the skin. Then add the over-the-counter antibiotic cream or the antimicrobial benzalkonium chloride-containing cream. Applying extra-absorbent powder or zinc oxide may also help.
Manage the pain. It may help to minimize swelling and alleviate pain by gently applying a wet, warm washcloth, tea bag or other forms of compress. For about 10 minutes, keep it on.
Ask your doctor to prescribe the pain medication that is most suitable. And speak to your doctor about how to dress and care for your wounds properly at home.
Stop tight clothing and products that are irritating. To minimize friction, wear loose, lightweight clothing. Some people notice that less contact with the skin is created by using tampons rather than sanitary pads. Using detergents and other non-perfumed, dye, and enzyme-free products.
Avoid the skin getting injured. Don’t squeeze the pimples and the sores, for example. bAnd avoid shaving infected skin.
Maintain healthy body weight and remain active. The symptoms of hidradenitis suppurativa can be made worse by not being at a healthy weight. Try to find activities that don’t make your skin irritable.
Consider having your diet changed. Diets that include dairy, red meat and foods with a high glycemic index can aggravate the symptoms of hidradenitis.
Stop all goods made from tobacco. Try to stop if you smoke. Symptoms of hidradenitis suppurativa can be exacerbated by smoking and other tobacco use.
Coping and support
Coping with discomfort and embarrassment can be one of the most serious difficulties of living with hidradenitis suppurativa. Your sleep, mobility or sex life may be impaired by painful sores.
They can smell if the sores are draining pus, despite good self-care. You may feel nervous, self-conscious or depressed, and become withdrawn.
Among your family and friends, try and find support. The concern and understanding of other individuals with hidradenitis suppurativa can also be comforting to you. Ask your doctor for a referral to a mental health provider or a support group’s contact details.
Planning your appointment
You can begin by seeing your doctor for primary care. He or she might refer you to a doctor (dermatologist) who specializes in treating skin diseases.
Your diagnosis can also include specialists in colorectal surgery, cosmetic surgery or digestive disorders (gastroenterology), depending on the seriousness of your condition.
To help you get ready for your appointment, here’s some stuff. What you should do for yourself. Create a list of the following things before your appointment:
Symptoms that you have experienced, including those that might seem unrelated to the reason you planned the appointment.
Both medications, vitamins and nutrients, including doses that you take.
Questions for your doctor
Some fundamental questions to ask your doctor for hidradenitis suppurativa include:
- What is the most probable cause of my symptoms, right?
- Are there any triggers that are possible?
- Am I in need of some tests?
- How long is my condition going to last?
- What are the available therapies, and which ones do you recommend?
- What side effects of treatment may I expect?
- Is another medical illness linked to this condition?
- Do you have any brochures that I can carry with me or other printed materials? What websites are suggested by you?
- What to expect from your physician
There are a variety of questions your doctor would possibly ask you, such as:
- When did your symptoms start?
- When they started, what did the skin lumps look like?
- Are they returning to the same spots?
- Are the signs unpleasant for you?
- Have your siblings or parents ever had this problem?
- What appears to help the symptoms, if anything?
- What seems, if anything, to make the symptoms worse?
- Do you smoke or use items made from tobacco?
Reference;