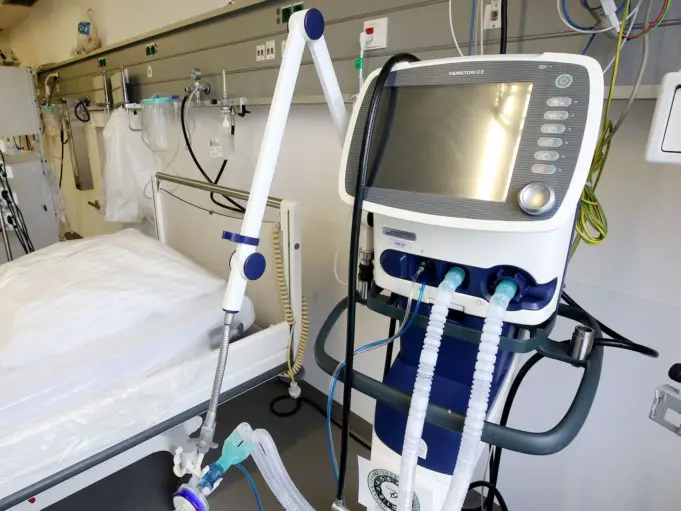
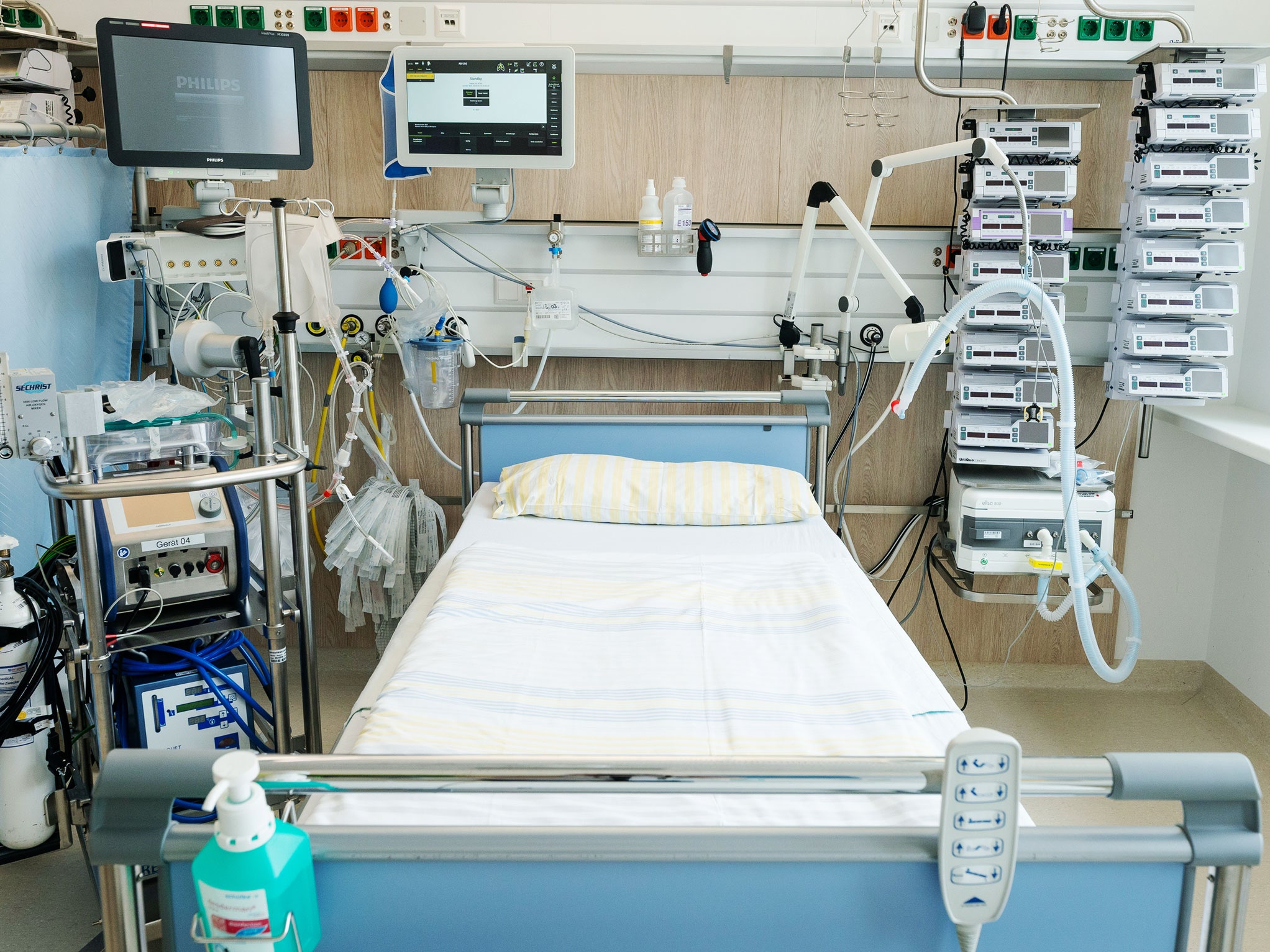
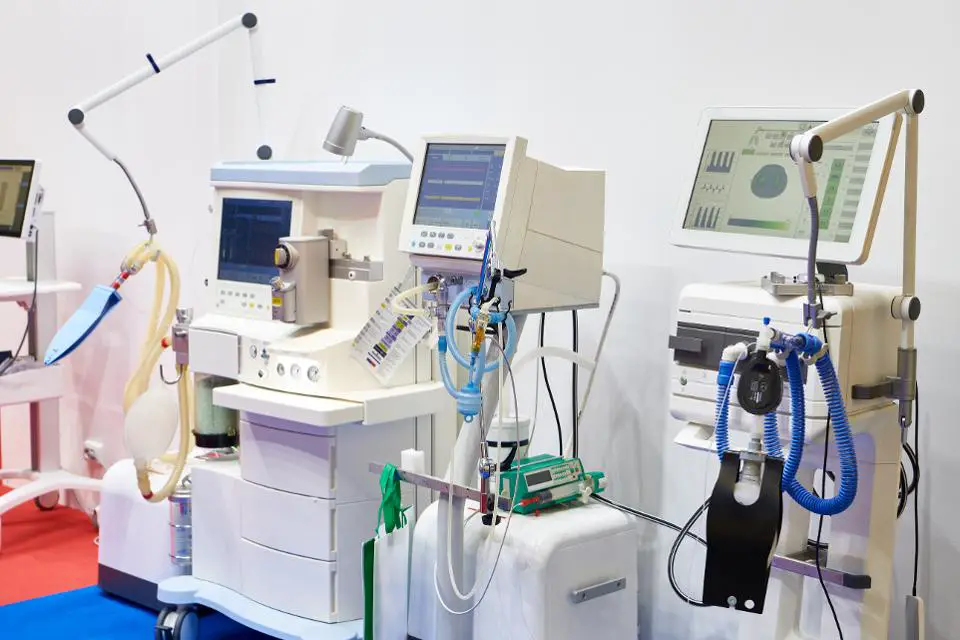
We sometimes find ourselves in situations where breathing becomes difficult or impossible, and thus the need for an emergency/artificial source of oxygen arises. This brought about the invention of ventilators.
Although considered as lifesaving, ventilators have some potential risk attached to them just like any other medical treatment.
What is a ventilator?
A ventilator is a machine commonly used in the medical field to aid respiration for people who find it very difficult to breathe.
The primary function of a ventilator is to calmly drive air in and out of the lungs when proper breathing is difficult. Although modern-day ventilators are mostly computerized machines, hand-operated bag valve masks can also serve as ventilators.
Common names of the ventilator include:
- Mechanical ventilation
- Respirator
- Breathing machine.
Ventilators can be used for babies, children, and adults when recovering from a sickness or other issue such as:
- Brain injury
- Drug overdose
- Coma or loss of consciousness
- Collapsed lungs
- Polio
- Lung infection
- Pneumonia
- Stroke
- Myasthenia gravis
- Guillain-Barre syndrome
- Chronic obstructive pulmonary disease (COPD)
- Upper spinal cord injuries
- Amyotrophic lateral sclerosis (ALS), commonly known as Lou Gerhig’s disease.
- Premature lung development ( in babies)
However, ventilators have also been used during the COVID-19 pandemic on some patients diagnosed with the disease, although this is for severe cases. The majority of people diagnosed with the disease will experience mild symptoms.
In conclusion, ventilators are mostly used in Intensive care units and during surgeries that require the use of anesthesia or after such surgeries where patients may find it hard to breathe on their own during the first few weeks.
How does ventilator work?
Basically, a ventilator works by pushing oxygen into the lungs and removing carbon dioxide from the body. A ventilator is made up of compressible air tanks, disposable patient circuits, air and oxygen supplies, and a set of valves and tubes.
The air tank is pneumatically compressed multiple times a minute so as to deliver an air/ oxygen mixture to the patient.
A breathing tube is connected from the ventilator to the patient. The way the end of the tube is connected to the patient differs depending on how critical the condition of the patient is.
The airways include the nose, throat(pharynx), mouth, lung tubes(bronchi), voice box(larynx), and windpipes(trachea). One end of the tube is connected to the lung airways through the mouth or nose for minor conditions. This is called Intubation.
For complicated conditions, the breathing tube is connected directly to the windpipe through a hole made in the neck by a minor surgical procedure; this process is called a tracheostomy.
Like every machine, a ventilator requires power to function. While some make use of direct electric supply, some respirators work with battery power.
Considering that the failure of a ventilator could result In the loss of life of the patient, ventilators are classified as life-critical systems. Thus, certain precautionary measures must be put In place to ensure that they are reliable, Including the area of power supply.
Ventilators are carefully built to avert danger on the life of the patient should any failure occur. They may have safety valves that open to the atmosphere to prevent suffocation and enable the spontaneous breathing of the patient.
Mechanical Ventilators could also have a backup mechanism to allow hand-driven respiration in the absence of power.
When is a ventilator necessary?
During surgery
Surgery requires anesthesia, which numbs all the muscles In the body, including the muscles that aids inhaling and exhaling, thus without the ventilator, breathing would be impossible during surgery.
During surgery, most patients are placed on a ventilator, and drugs are administered to them to stop anesthesia. Once the anesthesia is under control, the ventilator is removed, and patients can breathe on their own.
After surgery
The use of a ventilator might still be necessary after surgery because people sometimes need help to breathe a few hours or even a few days after surgery.
The inability of patients to breathe well after surgery may be a result of reduced lung function before the operation, which occurs when there is damage to the lung caused by chronic obstructive pulmonary disease (COPD).
Surgery sometimes requires that patients remain on the ventilator even after the surgery. For instance, patients who underwent open-heart surgery are needed to stay on the ventilator until they are fully awake and can perform some body movement, such as lifting their head from the pillow on their own.
Drugs are not administered to stop anesthesia; instead, it is allowed to fade away by itself, and then the ventilator is taken away from the patient to enable them to breathe on their own.
Long term care
Patients with critical and life-threatening conditions and are required to remain in the hospital for a more extended period may be put on a ventilator. However, the machine isn’t connected through their nostrils or mouth, but an opening is made in the neck of the patient.
This surgically created opening is known as a tracheotomy.
These patients are usually relocated to a Long Term Acute Care (LATC) facility where they will receive further treatment for a specific period of time or till they are strong enough to carry out essential functions like proper breathing.
Weaning
Weaning is the process of detaching someone from the ventilator. While some patients don’t have issues with getting off a ventilator, others might and detachment may take a while.
The ventilator is therefore adjusted to enable such patients to try to breathe on their own.
Risks of using a ventilator
Just like every other treatment, a ventilator could serve as a lifesaver, but it still has its side effects that pose a risk to human health.
Infections
Considering a tube would be connected to the windpipe from an external source, infections are one of the major risks a ventilator could pose to the patient’s health. Pneumonia and sinus infections are common cases amongst patients using ventilators.
Antibiotics are, therefore, necessary to treat these infections.
Irritation
The breathing tube can touch the throat or lungs of the patient, thereby causing irritation. It can also lead to patients having difficulty coughing. Coughing helps to rid off germs and dust in the lungs.
Immobility
Because most patients are subjected to sedatives, they don’t get to move around so much when using a ventilator. This can lead to bedsores, skin infections, and blood clots. Muscles, including those that aid breathing, may get also get weak.
Vocal cord problems
Breathing tubes pass through the voice box, thus making speaking impossible. The process of removing the tubes may lead to the vocal cords been damaged. Soreness and raspy voice are basic symptoms felt after the removal of the tube.
If you experience difficulty in breathing or speaking afterward, contact your doctor immediately.
Delirium
Due to heavy sedation and strong medications when using the ventilator, one may have a hard time reading, writing, or thinking even after the tube is removed because the medications may take time to wear off.
Poor memory, paranoia, and trouble sleeping are also possible effects.
Lung injury
Ventilator-Associated Lung Injury (VALI) is also a significant risk in the use of ventilators. Excess oxygen in the mix for too long can be very bad for the lungs. If the amount of air is too much or if the lungs are weak, it can damage lung tissues.
VALI can lead to some conditions, some of which are;
- Pneumothorax ( air leaks into space between the lungs and chest)
- Pulmonary edema
- Hypoxemia
What to expect on a ventilator
How you are monitored
Medical equipment that monitors your overall well-being will be needed while using a ventilator. You might need monitors for
- Oxygen saturation
- Heart rate
- Respiration rate
- Blood pressure
- Chest X-ray or scan
Additionally, you may blood tests to verify the amount of oxygen and carbon dioxide present in your blood.
Medications
While on the ventilator, your doctor might administer some drugs to help you feel more calm and relaxed. Those placed on a ventilator are usually given sleep medications,
- Pain medications
- Muscle relaxers
- Sedatives
These medications may cause drowsiness and confusion, with time it wears off, and you’ll no longer be needing them once you’re off the ventilator.
Things to look out for when disconnected from a ventilator
If you’ve been on a ventilator for a prolonged period, you may experience difficulty in breathing, sore throat, or aching chest muscles. This can be as a result of the ventilator performing the duty of your lungs and the drugs given to you while on the ventilator.
In some cases, your lungs and chest muscles may take a while to return to shape. Your doctor may, therefore, suggest that you undergo the weaning process.
You won’t be taken off the ventilator completely, rather the time which you are getting the ventilator support might be reduced. If, at any point, you developed pneumonia or any other infection from a ventilator, talk to your doctor immediately.
Conclusion
Ventilators are machines that aid breathing, they don’t fix health problems, but they sure help one breathe while the whole treatment procedure is being carried out.
How long a patient stays on a ventilator differs and is influenced by a lot of factors, including the ailment being treated, the patient’s respiratory system, and so much more.
Ventilators are lifesavers and can come in handy when treating babies or children whose respiratory system cannot handle vigorous treatments.