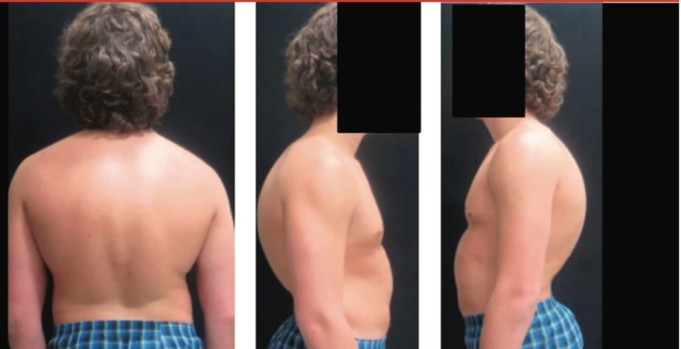
Scheuermann’s disease is simply a postural deformity; a spinal abnormality affecting the upper back, making the upper back rounded like a hunch.
It is also known as Scheuermann’s kyphosis, juvenile kyphosis, juvenile discogenic disease, adolescent kyphosis, or hunchback disease.
Scheuermann’s disease is a condition of hyperkyphosis that is characterized by an anterior curving of three or more vertebral bodies and a disc of the spine, the vertebral bodies are wedged greater than or equal to 5 degrees.
The thoracic vertebrae are mostly affected, although the thoracolumbar and lumbar vertebrae regions are sometimes involved as well.
Scheuermann’s disease is usually diagnosed in adolescents as from age 12 to 17 years who are presented by their parents or guardian after noticing a postural deformity or ‘hunchbacked’ appearance.
While the normal curvature of the upper spine (thoracic region) is between 20 to 50 degrees, a curvature greater than 50 degrees presents a Scheuermann’s disease condition.
It is accompanied by pain in the affected hyperkyphotic region and this is suspected to be the cause of initial evaluation. This condition related to the curvature of the spine was named after a Danish orthopedic surgeon and radiologist Holger Werfel Scheuerman (1877-1960), who was the first to describe the condition in 1920 as osteochondritis deformans juvenilis dorsi.
The condition is slightly predominant in males than females, occrung in approximately 5% of the general population. Scheuermann’s disorder is progressive and as the progresses, the curvature of the spine may become exaggerated and the individual will appear as if he/she is slouching or is very round-shouldered.
The etiology of Scheuermann’s disease is not certain but there is a hereditary component associated with this condition, although the exact mode of transmission is still not clear.
This is to be supported by the fact that the occurrence of Scheuermann’s disease is higher un monozygotic twins than dizygotic twins.
Causes of Scheuermann’s Disease
A definite and universally accepted cause of Scheuermann’s disease remains uncovered. As earlier stated in the article, a hereditary component is suspected to contribute to the disorder, but the mode of transmission is still unknown.
However, a developing theory, backed up by histological findings from conducted research suggests discordant vertebral endplate mineralization and ossification during growth which causes disproportional vertebra body growth and wedge-shaped vertebral bodies that lead to kyphosis.
This theory attributes the disease to metabolic, mechanical trauma to the growing spine or hormonal and nutritional deficiencies.
Scheuermann’s disease may also be influenced by spinal instability, which in turn is affected by ligament weakness and laxity. The spacing between the vertebrae is also affected.
Persons without this condition possess relatively uniform and rectangular-shaped spaces between their vertebrae but individuals with Scheuermann’s condition have spaces that become wedge-shaped.
Scheuermann’s disease usually lasts for six months to three years; any long-term effects are usually minimal, and if they do occur, they are usually helped with exercises.
Scheuermann’s disease is classified into type I, this the most occurring type of the condition, it involves the thoracic spine only with the apex of curve T7 to T9 and type II which involves both the thoracic and lumbar regions of the spine, with the apex of curve at T10 to T12.
Clinical Presentation and Symptoms of Scheuermann’s Disease
The symptoms of Scheuermann’s disease are very easy to notice during the growth of a child as the growth spurt that happen around puberty becomes obvious.
These signs include:
- A rounded, hunched back: it is sometimes more noticeable in some cases than others, kids are unable to stand properly, straightening their spinal curve. In other cases, the rounding might be difficult to identify.
- Back pain: This is very simultaneous with Scheuermann’s kyphosis onset.
- Inablilty to participate in physical exercise, work and other activities of daily living.
- Patient may have a negative cosmetic self-appearance due to presence of their deformity.
- A cutaneous skin pigmentation at the area of greatest curvature due to skin friction on chair backs.
- In serious cases, heart and lung function can be impaired or severe neurological symptoms can occur (these symptoms are extremely rare).
For a medical condition to be clinically called or presented as Scheuermann’s disease (kyphosis), it must have the following features:
- There must be no evidence of congenital, infectious or traumatic disorders of the spine.
- Three or more adjacent vertebrae must be wedged 5o or more.
The patient will show:
- Postural deformity
- Possible subacute thoracic pain, usually no identifiable inciting cause. The pain worsens during activities and subsides with rest.
- Physical exam shows rigid hyperkyphotic curve, accentuated with forward bending.
- Hyperhyphosis does not resolve with an extension or lying prone/supine, supporting the rigid nature of this deformity.
- Muscle stiffness and fatigue
- Decreased flexibility of the torso.
- Other associated findings on an examination might include cervical or lumbar hyperlordosis, scoliosis and tight hamstring.
Diagnosis of Scheuermann’s Disease
Physical examination of a patient’s medical history and radiographs is the essential components for evaluating Scheuermann’s disease.
Lateral radiographs are required for diagnosis and the condition must meet the following radiographic criteria:
- Thoracic spine kyphosis greater than 40 degrees (normal spine curvature is 25-40o)
- At least 3 adjacent vertebrae demonstrating wedging greater than 5 degrees.
Other associated criteria that are typical but not a necessity include
- Irregular vertebral endplates
- Schmorl nodes
- Loss of disc space height
- Disc herniation
- Scoliosis
- Spondylolysis
MRI (Magnetic resonance imaging) can assist to further evaluate anatomic changes or for pre-operative planning. CT (computerized tomography) imaging is usually not needed.
Physical examination may consist of:
- Postural assessment: examination of the posture from anterior, posterior and lateral view
- Neurological screening: rarely the spinal cord can be stretched over the posterior aspect of the vertebral bodies at the apex of the curvature which may cause neurological signs of impending paraplegia with clonus and hyperreflexia.
- Adam’s forward-bend test: Scheuermann’s disease can be accompanied by a scoliosis (a sideways curvature of the spine).
- Muscle length testing: the disease can be accompanied by tightness of the M. Pectoralis (most superficial bone in the pertoral region), M. Hamstrings, M. suboccipitalis and the hip flexors with possible contractures of the anterior shoulder and hip.
- Range of motion: flexibility of the extremities and spine can identify impairments and track changes over time.
- Muscle strength testing: strength of the abdominals, core, trunk extensors and gluteal muscles must be assessed.
Differential Diagnosis of Scheuermann’s Disease
Some few other spinal conditions may present similar symptoms with Scheuermann’s disease. Comparisons by clinicians and individuals may be useful for a differential diagnosis:
- Scoliosis
- Hyperkyphosis attributable to another known disease state
- Ankylosing spondylitis
- Postural kyphosis (flexible postural deformity)
- Postsurgicalkyphosis
Management and Treatment of Scheuermann’s Disease
When an adolescent is observed to have symptoms of Scheuermann’s disease, he/she is to see an orthopedist (a doctor who is a bone specialist).
The doctor will physically examine the spine, conduct an imaging test and recommend treatment.
Treatment options include:
Observation
When the rounding of the back is not likely to cause any problems, kyphosis may not need ant treatment. The patient will have routine checkups to ensure the rounding does not start causing problems. Most cases of Scheuermann’s disease will stop progressing when patients (kids) are done growing.
Back brace
This brace is like a jacket that can is worn under clothes and most effective in skeletally immature patients. It might not straighten the curve, but it will keep it from getting worse.
Some patients, especially younger patients (under 15) wear the brace only at night and others wear for 18-20 hours a day. These extension braces are usually recommended in kyphosis 60 to 80 degrees plus/minus symptomatic.
Bracing is typically required for 12 to 24 months until the kid stops growing. Some types include Milwaukee brace, Kyphologic brace, and Thoracolumbosacral orthosis-style Boston brace.
Surgery
This approach is not usually needed but doctors might recommend a procedure called spinal fusion for a severe case that causes pain or breathing trouble.
It is typically indicated in cases of kyphosis greater than 75 degrees causing unacceptable deformity, kyphosis greater than 75 degrees with associated pain, spinal compression, and severe refractory pain.
Physical therapy
Exercises that strengthen the muscles, lifestyle modifications and NSAIDs, in the back and core to support the spine better can sometimes aid the management of Scheuermann’s disease.
Majority of patients fall into this category and patients typically do well without significant long-term complications.
Other physiotherapy treatment might include:
- Postural improvement:
- Focuses on hamstring and pectoralis stretching and trunk extensor strengthening as well as improving function.
- These exercises can be effective when the thoracic spine has not developed a relevant stiffness and when the sagittal curve is not too high: Cobb angles from 44 to 55 degrees.
- Practice normal posture standing and sitting.
- Exercises:
- Flexibility exercises to relieve lower extremity contractures for example tightness of M. Hamstrings muscles.
- Strengthen core musculature, back extensors.
- Sports:
- Extension sports are advised, such as gymnastics, aerobics, swimming, basketball, and cycling and hyperextension exercises.
- Some sports should be discouraged like sports associated with jumping, marked stress and functional overuse of the back.
- Postoperative physical therapy:
- Necessary and must contain breathing exercises, mobilization and strengthening exercises, trunk elongation and expansion.
- Muscle activation by increasing tension: to achieve the best possible correction, muscle balance, stabilization and to increase the proprioceptive input. It helps to integrate the ‘corrected body schema’ in the brain.
Scheuermann’s disease in adults is regarded differently from that of the adolescents because the major manifestation is pain and not aesthetic quality.
The functional rehabilitation on an outpatient basis is the favored or choice treatment but referral for surgery or dorso-lumbar braces is rare. More clinical are however necessary to evaluate the effectiveness of conservative interventions, especially different exercises and manual therapies.
These should be combined with braces.
Complications
The adventitious circumstances or conditions that might coexist or modify the existence of Scheuermann’s disease come from the symptoms.
Some potential complications of Scheuermann’s disease include Progressive cosmetic deformity, chronic back pain, neurologic deficits (spinal cord compression) and some postoperative complications also include persistent pain and peudoarthrosis (most common complication).
Patient Education on Scheuermann’s Disease
Scheuermann’s disease require important patient education, these include:
- Extension-based stretching/strengthening program.
- Proper postural and body mechanic techniques for ADLs
- Hamstring stretching exercise program.
- Appropriate use and handling of braces.
Summary
For surgical patients, in-patient rehabilitation might be necessary for mobility and strength training as well as aggressive postoperative pain management.
Consultations, although not always a necessity, it is good practice for any patient with some degree of suspected spinal deformity to establish care with either an orthopedic spine surgeon or neurosurgeon.
Orthopedic spine surgery consultation should be obtained for any Scheuermann’s disease patient with the following any neurologic deficit and patients with compromised pulmonary function testing attributable to their kyphosis.
Sources;
- Symptoms and Diagnosis of Scheuermann’s Disease; https://www.spine-health.com/conditions/spinal-deformities/symptoms-and-diagnosis-scheuermanns-disease
- Scheuermann’s Disease; https://www.gillettechildrens.org/conditions-care/scheuermanns-disease
- Scheuermann’s Disease;https://www.humpalphysicaltherapy.com/Injuries-Conditions/Upper-Back-and-Neck/Upper-Back-Issues/Scheuermann-s-Disease/a~5944/article.html
- Scheuermann’s Disease; https://en.m.wikipedia.org/wiki/Scheuermann%27s_disease