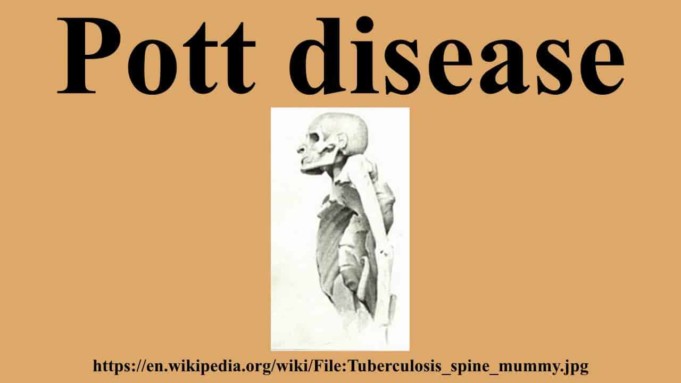
Pott’s disease goes by many other names but the most medical term for this condition is tuberculous spondylitis or tuberculosis of the spine.
Pott’s refers to vertebral body osteomyelitis (infection of the bone) and intervertebral diskitis (infection in the intervertebral disc space) from tuberculosis (TB).
Pott’s disease is a disease caused by the infection of the spinal column by a tuberculosis bacillus, Mycobacterium tuberculosis. This disease results in the softening and collapse of the vertebrae, causing the affected individual to have a hunchback curvature of the spine, a condition commonly termed Bone tuberculosis.
The Bacteria Tuberculous bacilli have for a very long time lived symbiotically with man since the evolution of Homo sapiens on Earth. As far back as before 1,000 BC, the symptoms and communicability of tuberculosis have been known to man.
Ancient pathological proofs of bone tuberculosis including joints and spines in prehistoric humans have also been recorded. In ancient India, the Rig Veda and the Atharva Veda (3500-1800 BC) mention this disorder by the name Yakshama in all its forms.
Pott’s disease was first described in 1779 by Percivall Pott. He described the condition in a published monograph as an infection that begins in the body of the vertebra; the most common site of bone tuberculosis and spreads slowly to a contiguous structure.
Abscesses may form and drain into soft tissues adjacent to the spine, resulting in pains in the site distant from the infection. Pott’s disease is one of the most frequent bacterial infections that affect the spine in countries where tuberculosis is prevalent.
And research data shows that the incidence of Pott’s disease specifically in developing countries, as with other forms of TB, is on the rising side due to new multiple drug-resistant strains.
Diskitis and osteomyelitis comprise approximately 50% of all musculoskeletal tuberculosis and usually affects the lower thoracic and upper lumbar levels of the vertebra column.
Nature of Pott Disease
Due to hematogenous spread through the venous plexus of Batson, the spine is usually affected. When affected, there is a slow collapse of one or more vertebral bodies, which spreads underneath the longitudinal ligaments.
This spread result in an acute gibbus or kyphotic deformity.
This angular formation, coupled with epidural granulation tissue and bony fragments, can lead to a chord compression. Unlike other bacterial infection that forms pus, the disc can persevere, and this infection commonly involves the thoracic spine.
In late-stage Pott’s disease, large paraspinal abscesses without pain or frank pus are common.
Causes of Pott’s Disease
The name of the bacteria that causes Pott’s disease is known as Mycobacterium tuberculosis.
The way this bacterium gets to the spine is hematogenously from an outside spinal site of infection, for instance, the lungs using the lymphatic system as the vessel of transmission.
This is a common site of transmission in adults but in children, the site is unknown. Once it gets to the vertebral column, the bacterium can attack the vertebrae, intervertebral discs, the epidural or interdural space within the spinal canal, and adjacent soft tissues.
When the infection develops, it distributes itself across the vertebral column, infecting the posterior and anterior longitudinal ligaments and the periosteum from the front and sides of the vertebral bodies.
The end result is loss of the periosteal blood supply and detachment of the anterolateral surface of the vertebrae. If only one vertebra is affected, the surrounding intervertebral disc will not be affected.
But if two adjacent vertebra bones are affected, the intervertebral disc between them collapses and becomes avascular (lacking blood vessels).
Spinal collapses which are one of the most common visible symptoms of Pott’s disease are caused when cavities formed from dead tissues, usually filled with pus (abscesses) forms in sites near the vertebral column (paravertebral).
These paravertebral abscesses can also develop calcifications or sequestra within them, forming what is known as cold abscesses. These abscesses when formed in the lumbar region may descend down the sheath of the psoas to the femoral trigone region and eventually erodes into the skin.
Symptoms of Pott Disease
Persons suffering from Pott’s disease, during the early onset of the disease, usually complain of pains during movement and with time their bodies assume a protective, stiff position.
Pott’s disease runs s slow course, lasting for months or even years. In addition, the disease in few cases, tuberculosis dominant in the lungs can spread without the patient knowing they have any form of tuberculosis at all.
But once a person contracts bone tuberculosis, he/she might experience severe back pain, swelling, stiffness, and abscesses.
Major characteristics or clinical presentations of Pott’s disease include:
Spinal Involvement
- About 15% of Pott’s disease cases involve the cervical spine
- The lower thoracic vertebrae are the most common area of involvement (40%-50%) followed by the lumbar spine (35%-45%). The thoracic spine is involved in about 65% of cases, and the lumbar, cervical, and thoracolumbar spine in about 20%, 10%, and 5% respectively.
- The atlantoaxial region may also be involved in less than 1% of cases.
Physical Findings
- Spinal deformity
- Neurological deficits
- Muscle spasms
- Localized tenderness
- Restricted spinal motion
Back Pain
This is the earliest and most common symptoms of Pott’s disease. Patients who suffer from the condition usually experience back pain.
This pain caused by spinal tuberculosis can present as spinal or radicular.
Spinal Deformities
Almost 90% of patients with Pott’s disease have some issue of spinal deformity with thoracic kyphosis being the most common.
Neurological Signs
Pott’s disease involves spinal cord compression with the following:
- Paresis
- Impaired sensation
- Paraplegia
- Nerve root pain
- Cauda equine syndrome
Constitutional Symptoms
- Fever
- Weight loss
- Malaise
- Night sweats
Associated Co-morbidities
- Peptic Ulcer
- TB
- HIV/AIDS
- Alcoholism
- Malnourishment
- Low Socio-economic status
- Gastrectomy
- Drug addiction
- Immunosuppressive Disorders
Diagnosis of Pott’s disease
Tests conducted to confirm Pott’s disease and rule out other medical disorders with similar features include:
- Blood tests
- Elevated erythrocyte sedimentation rate: >100mm/h
- Complete blood count: To check for raised white blood cell count (leukocytosis)
- Radiographs of the Spine: changes of the spine radiographically associated with Pott’s disease usually present itself relatively late. On a plain radiograph, the following are the features of spinal tuberculosis:
- Increased anterior wedging.
- Lytic destruction of anterior portion of vertebral body
- Collapse of vertebral body.
- Enlarged psoas shadow with or without calcification.
- Reactive sclerosis on a progressive lytic process
- Vertebral endplates are osteoporotic.
- Vertebral bodies show varying degrees of destruction.
- Intervertebral disks may be shrunken or destroyed.
- Fusiform paravertebral shadows suggest abscess formation.
- Bone lesions may occur at several levels of the spine.
- Bone Scan
- Computed Tomography of the spine
- Bone Biopsy
- MRI
Treatment of Pott’s disease
When treated early enough with the right regimen of medications, the painful side effects of Pott’s disease and damages can the reversed.
Surgery may be necessary as seen in many cases, such as Laminectomy (where a part of the vertebrae is removed) is common.
A treatment goal for every approach to Pott’s disease is to:
- Eradicate infections.
- Confirm diagnosis.
- Identify and Remove Causative Pathogen
- Maintain/Recover Neurological Function
- Maintain/Recover Mechanical Stability of Spine
- Returning Functional Activities to Daily Life
- Prevent Spinal Deformity and Possible Sequelae
The time to complete treatment is very controversial, although some studies favor 6 to 10 months courses, traditional courses range from 9 months to as long as 14 months.
The duration of therapy is individualized and base on the resolution of active symptoms and clinical stability of the patient. The drugs used during treatment are classes that consist of agents that inhibit the growth and proliferation of the causative bacteria.
Treatment techniques used on Pott’s disease depending on the severity of the condition, cause of the disease, and diagnosis, some these techniques include:
- Surgical drainage of abscesses
- Anti-Tuberculosis chemotherapy
- Surgical decompression of the spinal cord
- Spinal immobilization
- Surgical spinal fusion (Laminectomy)
These medications possess different during in the course of treatment, for instance, Isoniazid and rifampin should be administered during the whole course of therapy, additional medications are administered during the first two months of therapy and these are carefully selected among the first-line drugs which may include ethambutol, pyrazinamide, and streptomycin. The second line of drugs consists of drugs indicated in cases of drug resistance.
Some conditions can serve as good indicators of response to the possible treatment of Pott’s disease; with these conditions, doctors can be 70% sure of positive response to treatments:
- Good general condition
- Partial cord compression
- Short duration of neural complications
- Young age
- Early onset cord involvement with delayed neural complications
Management of Pott’s disease After Surgery
Post-surgical Treatment administrations should be addressed individually, focusing on any impairment, functional limitations, and disability outcome.
Pott’s disease Post-spinal decompression treatment management involves;
- Spinal stabilization exercises
- Back school
- Exercises and strengthening
When compared, spinal stabilization was found to produce significantly positive results and has highest global ratings.
Pott’s disease management after Post-spinal fusion surgery involves:
- Transcutaneous Electrical Neuromuscular Stimulation (TENS)
- Aquatic therapy
- Aerobic exercises
- Trunk strengthening
- Overground training (walking program)
Research reveals that management with TENS has a higher frequency of effectiveness in decreasing neuropathic pain. However, others also show interventions in attaining significant decreases in pain, disability, and psychological distress.
Summary
Effective and efficient chemotherapy for Pott’s disease is a very good start for the fighting spreading of Pott’s disease and it must be started at the early stages of the disease.
Patients have a 95% chance of recovery without significant deformities and complications if the diagnosis is made at the pre-destructive stage and the patients are treated with standard drugs.
Although neural complications are still encountered in general hospital outpatients, diagnosis and treatment at early stages would resolve the neurology without operation in about 40% of cases.
Sources;
- Tuberculosis Spondylitis; http://radiopaedia.org/articles/tuberculous-spondylitis-2
- Pott Disease; http://britannica.com/science/Pott-disease
- Pott Disease; https://en.m.wikipedia.org/wiki/Pott_disease