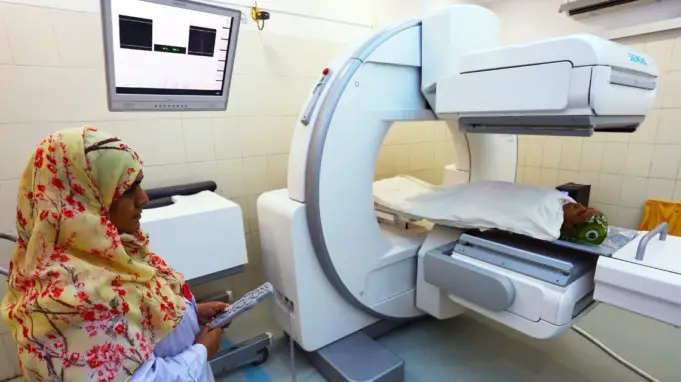
Nuclear medicine is a specialised area of radiology that utilises minimal amounts of radioactive materials, or radiopharmaceuticals, to examine organ function and structure, diagnose and treat illnesses, and radiation is used in nuclear medicine.
In nuclear medicine, radioactive materials known as radiopharmaceuticals or radioisotopes, are introduced into the body. In radiology, X-rays enter the body from the exterior.
While radiation can be dangerous at higher levels and concentrations, radioactive which are a particular type of radiation has been essential to the development of contemporary medicine. Doctors use it for a vast range of things, from examining a broken toe to treating cancer.
The use of radiation and radioactive in medicine, especially for diagnosis (identification) and therapy (treatment) of various medical conditions is widely known. In advanced countries, about one person in 50 utilises diagnostic nuclear medicine annually.
Nuclear medicine utilises radiation to gather information about the performance of specific organs in the body or to treat an ailment. In some cases, the information is used by physicians to diagnose the patient’s illness.
The liver, heart, bones thyroid, and many other organs can be easily imaged, and malfunction revealed. In other cases, radiation can be used to treat organs riddled with diseases and tumours.
Five Nobel Laureates are involved with the study of the use of radioactive tracers in medicine.
Nuclear medicine diagnosis
Radioisotopes are an important part of medical diagnostic procedures. In addition to imaging devices which register the gamma rays discharged from within, they can examine the dynamic processes taking place in the organs of the body.
Worldwide, 10,000 hospitals use radioisotopes in medicine, and about 90% of the procedures are used in diagnosis. A common radioisotope used in over 40 million diagnosis procedures annually is technetium-99 (Tc-99), it accounts for over 80% of all nuclear medicine procedures and 85% of diagnostic scans in nuclear medicine worldwide.
In developed countries (26% of the world population) the frequency of diagnostic nuclear medicine is 1.9% per year, and the rate of therapy with radioisotopes is about one-tenth of this. Physicians developed Nuclear medicine in the 1950s with an endocrine emphasis, initially use iodine-131 to diagnose and treat the thyroid disease.
When using radiopharmaceuticals for diagnosis, a radioactive dose is administered to the patient, and the activities of the organ can then be studied either as a two-dimensional picture or, using tomography, as a three-dimensional image.
Diagnostic techniques in nuclear medicine utilise radioactive tracers which emit gamma rays from within the body. These tracers are typically short-lived isotopes connected to chemical compounds which allow specific physiological processes to be investigated.
It may be administered orally, and it can be injected, or inhaled. The earliest technique developed uses one photon discovered by a gamma camera which can display organs from different angles.
The camera develops an image from the angle from which radiation is discharged; this image is improved by a computer and viewed on a monitor for indications of abnormal conditions.
Single-photon emission computerised tomography (SPECT) is the latest significant scanning technology to diagnose and observe a wide assortment of medical conditions.
A recent discovery is positron emission tomography (PET) which is a more accurate and technologically advanced technique using isotopes produced in a cyclotron. A positron-emitting radionuclide is administered, usually by injection, and assemble in the target tissue.
As it deteriorates, it emits a positron, which promptly connects with a closeby electron leading to the concurrent emission of two identifiable gamma rays in opposite directions. They can be picked up by a PET camera and given specific indications of their origin.
PET’s most significant clinical role is in oncology, with fluorine-18 as the tracer, since it has established to be the most precise non-invasive method of detecting and assessing most types of cancers. It can also be used in cardiac and brain imaging.
New procedures integrate PET with computed X-ray tomography (CT) scans to give co-registration of the two images (PET-CT), which gives 30% better diagnosis than a traditional gamma camera alone.
It is an important and efficacious tool which provides unique information on different variety of diseases from dementia to cardiovascular disease and cancer.
The positioning of the radiation source within (rather than external to) the body is the fundamental difference between nuclear medicine imaging and other imaging techniques such as X-rays.
Gamma imaging by any of the method described provides a view of the position and concentration of the radioisotope within the body. Organ malfunction can be spotted if the isotope is either partially taken up in the organ (cold spot), or taken up in excess (hot spot).
If a sequence of images is taken over some time, an unusual pattern or rate of isotope movement could indicate a malfunction in the organ.
Distinct importance of nuclear imaging over X-ray techniques is that both bone and soft tissue can be imaged very successfully. This has resulted in its frequent use in technologically advanced countries where the probability of anyone doing such a test is about one in two and rising.
Radiation constitutes an integral part of modern medicine, which includes radiation therapy, scans and imaging.
Radiation happens when an object or body gives off energy that travels in a straight line through a material or through space which moves in waves and forms a spectrum of longer to shorter waves.
The shorter the wave is, the higher the energy is. The absorption of radiation by human tissue is measured in greys (Gy). This absorption is a dose. When examining the risk of exposure to radiation, they use millisieverts (mSv).
These units help Doctors and scientists keep radiation within safe and acceptable limits while using them to diagnose and treat health problems.
Use in medical imaging
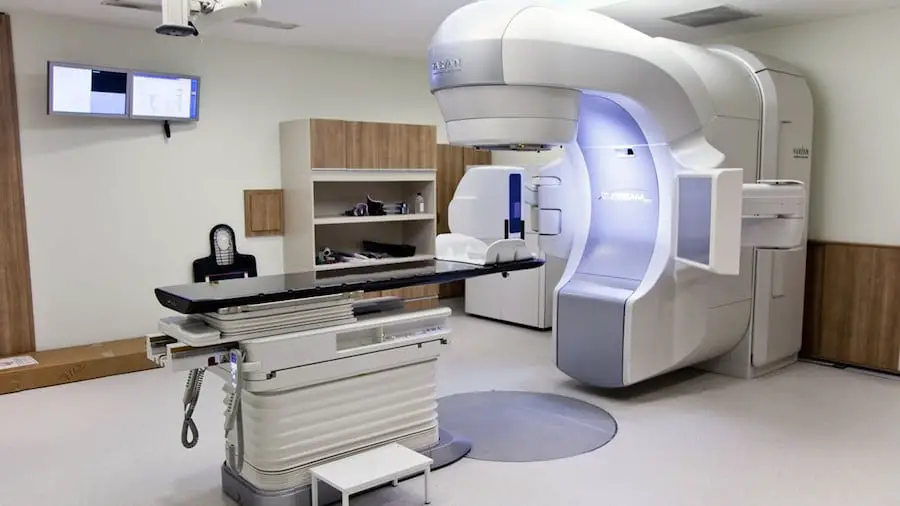
In healthcare, medical professionals use radiology to diagnose diseases using radiation-based imaging technologies.
Projectional radiography can help get an image of a body part. These techniques include:
- X-rays
- Fluoroscopy
- CT scans
- Ultrasound
- MRI scans
X-ray
The radiologist, or X-ray technician, directs the ray to a part of the body, which absorbs some of the radiation.
Hard tissue, like the bone, tooth enamel etc. absorbs more radiation than soft tissues, including muscle and cartilage. The remaining X-rays pass through the body and expose photographic film on the other side, creating a shadow effect.
Different parts of the body require different strengths of X-ray. Doctors commonly use X-ray for examining the chest, in mammography, and on limb fractures.
Fluoroscopy
Fluoroscopy utilises X-rays and a contrast material, usually iodine or barium, to get a moving image of what is happening inside the body.
Examples include angiography, for viewing the heart and blood vessels, and gastrointestinal fluoroscopy, which lets physicians see the digestive tract.
CT scan
A CT scan makes use of X-rays and computers to show parts of soft and hard tissues. They will often incorporate contrast agents or dyes that make the image clearer. CT scans provide a 3D impression of a part of the body.
Uses of CT scans comprise using it to look for an injury in the brain and examining for appendicitis in the abdomen, among many other things.
Ultrasound
Ultrasound utilises high-frequency sound waves to see soft tissues like the muscles, tendons etc. inside the body. Sound waves do not produce ionising or potentially damaging radiation that the body can absorb.
Ultrasound scans can show images in real-time, and its use is gradually expanding. They can provide people with an image of their child during pregnancy or guide surgical procedures for improved accuracy.
Doctors use ultrasound increasingly often at the bedside to assist with a range of procedures, such as extracting fluid from the lungs, known as pleural effusion, or evaluating for a tear in the rotator cuff of the shoulder.
Magnetic resonance imaging (MRI)
An MRI machine uses non-ionising radiation to produce high-quality images. Magnetic resonance imaging (MRI) utilises strong magnetic fields and a radio signal to take high-quality 3D images of the body.
The individual has to lie very still in a mildly noisy tube for an extended period, and this experience can be uncomfortable. However, the scan provides excellent images of soft tissue.
MRIs do not use any damaging ionising radiation, only strong magnetic fields and non-ionising radio frequencies. MRI provides high-quality images of muscles, tendons, and ligaments. In the brain, an MRI can identify the difference between a tumour and an aneurysm.
DEXA scan
Doctors use dual-energy X-ray absorptiometry (DEXA), or bone densitometry, to examine for osteoporosis.
DEXA scans make use of two narrow X-ray beams to measure the density of the bone. They do not produce images, so this scan is not a type of projectional radiography.
PET scan
A positron emission tomography (PET) scan is a radiation imaging technique in Nuclear medicine that requires the injection of a radioactive contrast agent, or tracer, into the body.
This tracer radioactively deteriorates in the body and emits positron particles. The PET scanner picks up these particles, and the Doctor or technician then uses a computer to reconstruct 3D images.
A PET scan picks up chemical activity in the body, and it is helpful in the surveillance of various types of cancers. It can also indicate blood flow in the heart, and it can help highlight information about neurological conditions such as Alzheimer’s and seizures.
Use in medical treatment
Many of the imaging techniques are used in treatment as well as diagnosis. Ultrasounds and X-rays can be used to guide biopsy procedures, and ultrasound is used to break down kidney stones, making them easier to excrete.
Radioactive procedures can also be used in treating conditions. The same radioisotopes that are used in imaging can be used to treat. The radiopharmaceutical can be taken orally, injected, or inhaled.
One instance is radioactive iodine (I-131) which has been used for over 50 years in treating thyroid cancer and hyperthyroidism, or hyperactive thyroid. Recently, it has also been used in treating bone pains from some types of cancer and non-Hodgkin lymphoma.
Iodine-131 (I-131) targeted radionuclide therapy (TRT) administers radioactive iodine into the body. As the thyroid cells or cancer cells assimilates this substance, it destroys them. I-131 can be administered in pill or in liquid form.
Experts in biomedical engineering, nanotechnology, advanced polymer chemistry, and molecular biology are examining ways to deliver the drugs to the right site without affecting surrounding tissues.
It is speculated that in the nearest future, it will be practicable to embed chemotherapy into medication imaging agents that will attach solely to cancer cells. Consequently, the chemo would destroy only the target cells without harming the healthy tissue. This would cut down most of the adverse effects of chemotherapy.
Radioimmunotherapy (RIT) infuse nuclear medicine (radiation therapy) with immunotherapy. Immunotherapy is a procedure that copies cellular activity in the body.
Combining the two types of treatment means nuclear medicine can be targeted more directly to the cells that need it. Radionuclidesof different forms are used. The commonest of them is I-131 or radioactive iodine therapy (RAI).
Other types are 90Y-ibritumomab tiuxetan, or Zevalin, which is used in treating different types of lymphoma. 131-I-tositumomab or Bexxar can also treat lymphoma and multiple myeloma.
Theranostics combines nuclear medicine techniques for treatment with those fo diagnoses and imaging. By integrating molecular targeting direction, such as peptides, with radionuclides, it can direct the radioactive substance to the target area to diagnose and deliver treatment at the same time.
Sterilisation
Gamma rays can be used to sterilise many medical products. Recently many medical products are sterilised by gamma rays sourced from a Co-60, a process which generally is more effective and cheaper than steam heat sterilisation.
The disposable syringe is an example of medical products that can be sterilised by gamma rays. Because it is ‘a cold’ process radiation can be used to sterilise a lot of items that are heat sensitive such as solution, powders, and ointments, as well as biological preparations such as blood, skin, nerve, and bone.
Large-scale irradiation facilities for gamma sterilisation are installed in many countries. Smaller gamma irradiators, often utilising Cs-137, having a longer half-life, are used for treating blood for transfusions and other medical applications.
Sterilisation by radiation has plenty of benefits. It is cheaper and more effective because it can be done after the item is packaged. The sterile shelf-life of the item becomes indefinite provided the seal is not broken.
Apart from syringes, medical products sterilised by radiation include cotton wool, burn dressings, surgical gloves, heart valves, bandages, plastic, and rubber sheets and surgical instruments.
What to expect from Nuclear medicine
An individual’s experience of Nuclear medicine using radiation will depend on several factors, including the type and location of cancer. Radiation treatment for oesophagal cancer, for example, can make eating difficult due to its effects on the food pipe.
Sit down with the treating Doctor and look over all the options available. Other types of Nuclear medicine involve swallowing a radioactive isotope as a liquid or a capsule, such as when treating thyroid cancer.
Alternatively, a doctor may inject radioactive isotopes into the spaces near the damaged body part. Radioactive iodine often plays a role in thyroid cancer treatment.
Researchers are looking into ways of improving Nuclear Medicine. In particular, they are investigating more selective treatments that can specifically damage cancer cells while sparing healthy cells.
A single x-ray typically uses a minimal amount of radiation to create an image of a part of the body. Exposure to the x-ray itself is unlikely to have any short-term side effects, though if you have to ingest or inject contrast for a scan, you might react to it. X-rays are generally safe for most people.
However, ask the Doctor if one has any concerns about getting an X-ray. People who are pregnant should also consult a doctor to find out what type of imaging test is best for them.
According to research by the Center for Nuclear Science and Technology Information, about one-third of all medical procedures in modern hospitals use nuclear medicine. The methods offered are effective, safe, and painless, and they do not need anaesthesia.
A radiologist is a doctor who specialises in radiology. Nuclear medicine can be used to diagnose a wide variety of conditions. In this mode of treatment, a patient can be made to inhale, swallow, or be injected with a radiopharmaceutical.
This is a radioactive material. After taking the substance, the patient will typically lie down on a table, while a camera takes pictures.
The camera will be focused on the area where the radioactive material is concentrated, and this helps the Doctor discern what kind of a problem there is, and where the problem is. Positron emission tomography (PET) and single-photon emission computed tomography (SPECT) are types of imaging.
Doctors and Health personnel use PET, and SPECT scans to get accurate information about how a body organ is working.
This type of imaging can be specifically helpful in diagnosing thyroid disease, gallbladder disease, heart conditions, and cancer. It can also aid with diagnosing Alzheimer’s disease and other types of dementia and neurological conditions.
Formerly, diagnosing internal conditions necessitates surgery, but nuclear medicine makes this practice obsolete. When treatment begins, PET and SPECT can be used to track progress, and SPECT can also offer fresh insights into addictions, cognitive conditions, and neurological disorders.
Other types of imaging involved in nuclear medicine can include targeted molecular ultrasound which plays a role in diagnosing cancer and metabolic disorders and can be helpful in magnetic resonance sonography, diagnosing different types of cancer, and highlighting blood flow.
What to expect
A person going for nuclear medicine treatment or diagnosis is advised to inform the health professional or doctor if they are pregnant, suspect they could be pregnant or nursing a child.
Nuclear imaging
The patient will have to wear a gown, or they might be able to wear their clothes, but they will have to remove the jewellery and other metal-base accessories.
Therapy
- After having radioactive treatment, the patient might have to take time off work and other social activities as they have to avoid physical contact with other people as much as possible for 2-5 days.
- When a patient receives radioactive treatment for the thyroid with I-131, no special equipment is employed.
- A single, one-time treatment prepared dose will be taken orally.
- The patient would be advised not to eat or drink after midnight on the day of the treatment. If the procedure is for a thyroid problem, the Doctor will generally recommend them to stop taking their thyroid medication 3 and 7 days before treatment.
- The patient might be allowed to return home after treatment, or they may have to say in the hospital overnight.
- However, the body will not absorb all the radioactive iodine, and it will remain in the organ for 2 to 5 days.
- This may mean taking time off work. They should also prepare their food, avoid sleeping with another person, flush the lavatory twice after use, and wash their clothes and laundry separately.
- Most of the iodine will leave the body through the urine, but it is also excreted through tears, sweat, saliva, vaginal discharge, and faeces.
- Women should avoid becoming pregnant for 6 to 12 months following treatment.
- Anyone who plans to travel immediately after treatment should get a letter from the Doctor, as radioactivity may show up on scanning machines at airports.
Safety in nuclear medicine
Too much radiation can potentially damage organs or tissues or increase the risk of cancer. However, when used for diagnosis, the level of radiation exposure is around the same as a person receives during a routine chest x-ray or a CT scan.
As a result, nuclear medicine and imaging procedures are considered non-invasive and relatively safe. Their effectiveness in diagnosing disease means that the benefits typically outweigh the risks.
Treatment with nuclear medicine involves more substantial doses of radioactive material. For example, a nuclear medicine lung scan would expose a person to 2 millisieverts (mSv) of radioactivity, while cancer treatment would expose a tumour to 50,000 mSv.
This additional dose may affect the patient, and side effects are possible. However, since the treatment often targets potentially fatal diseases, the benefits tend to outweigh the risks.
As technology advances, scientists hope that treatments will be more directed toward the tumour or disease, and less likely to affect the person as a whole.
The Nuclear Regulatory Commission (NRC) and the U.S. Food and Drug Administration (FDA) strictly regulate the use of radioactive materials for nuclear medicine to ensure the safety of patients.
References;
- What is nuclear medicine?; Medical News Today
- Nuclear Medicine; Hopkins Medicine
- Radioisotopes in Medicine; World Nuclear