Mansonellosis is a disease caused by three species of filarial parasites – Mansonella perstans, Mansonella streptocerca, and Mansonella ozzardi.
These filarial (nematode) parasites use humans as their definitive hosts. They are transmitted from one person to another by bloodsucking females of two families of flies known as Diptera and Ceratopogonidae (Biting midges).
These flies are known to transmit all mansonella species, but only black flies (Simuliidae) are known to play a role in the transmission of Mansonella ozzardi in parts of Latin America.
Mansonella perstans
This parasite is transmitted via the bites of midges and is endemic in parts of sub-Saharan Africa and the Americas. It has been estimated that over 100 million people are infected globally.
Unsheathed microfilariae of the species are found in the bloodstream while adult worms reside in the pericardial, pleural and peritoneal cavities. Midges acquire these worms when they take a blood meal from an infected human host.
M. perstans infections are often asymptomatic or mild. Adult worms can cause swelling similar to those of Loa loa. Inflammation of the pericardium, periocular inflammation, retinal damage as well as general malaise may also occur.
Diagnosis is made by identifying non-sheathed microfilariae in a blood smear. The parasite is relatively resistant to medication used to treat other filarial diseases.
Mansonella ozzardi
M. ozzardi is a filarial parasite endemic in Central and South America and several Caribbean islands. Humans are the primary hosts of the parasites, which are transmitted by biting midges and blackflies (Simulium amazonicum).
Although it has similar life cycles to that of M. perstans, adult worms reside in the lymphatic nodes as well as thoracic and peritoneal cavities. Microfilariae exist in both the blood and skin.
Most people infected with M. ozzardi often show no symptoms. However, some may have arthralgias, fever, skin rashes, lymphadenopathy, pulmonary symptoms and headache.
Diagnosis of the parasite is confirmed by identifying microfilariae in blood or skin samples. Treatment of mansonellosis caused by M. ozzardi is with ivermectin.
Mansonella streptocerca
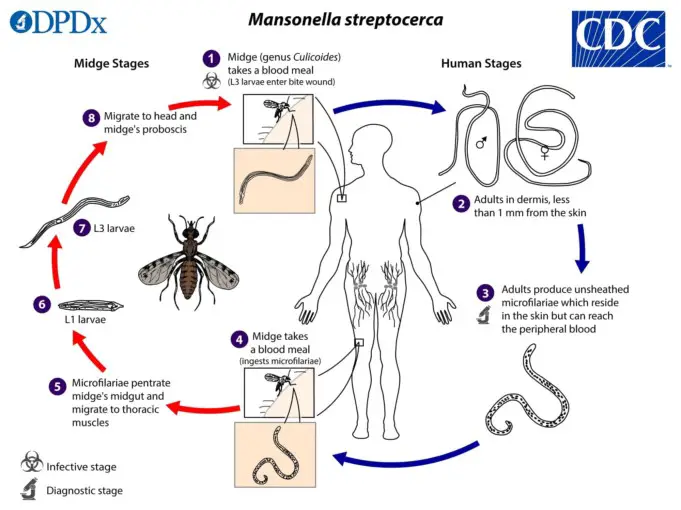
M. streptocerca is endemic to tropical rainforests in the west and central Africa and Uganda. Nonhuman primates are occasionally infected but are not the main reservoirs of the infection.
The life cycle of Mansonella streptocerca is similar to that of M. perstans except adult worms reside in the dermis of the shoulder areas and upper trunk.
Microfilariae are found in the skin. Mansonellosis caused by M. streptocerca is asymptomatic although thickening of the dermis may be observed.
The diagnosis is made by identifying microfilariae in skin snips or biopsies. Diethylcarbamazine (DEC) 2 mg/kg orally three times a day for 12 days is used to treat Mansonella streptocerca.
DEC eliminates both microfilariae and adult worms. It can, however, worsen skin and systemic symptoms due to the release of antigens from the dying microfilariae.
The drug should not be administered to patients with heavy Loa loa or concurrent O. volvulus infections due to the potential for severe adverse effects.
Sources
- Centers for Disease Control and Prevention – Mansonellosis
- MSD Manual – Mansonellosis