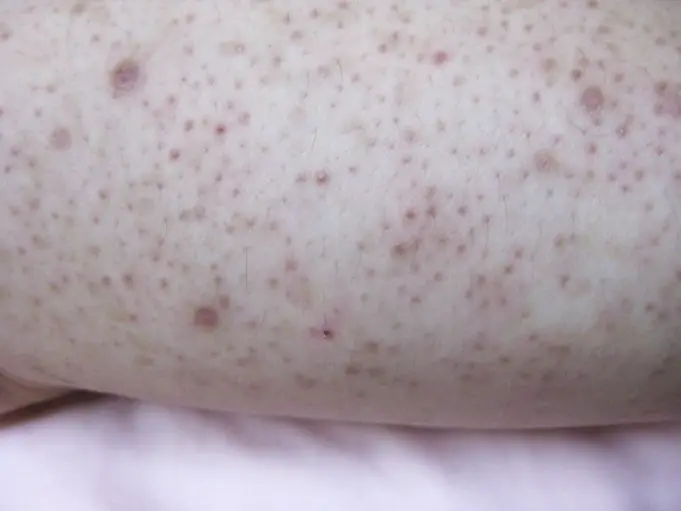
Keratosis pilaris is a skin condition characterized by small, inflammatory, irritation spots on the skin. It is similar in appearance to a pimple but without pus.
Keratosis pilaris is listed among the most frequent dermatologic conditions (skin conditions) and is somewhat considered a standard variant.
The other names for Keratosis pilaris include Follicular keratosis and Lichen pilaris. It is the most common follicular keratosis in both adults and adolescents.
Keratosis pilaris is harmless and controlled by many factors, affecting the proximal extremities’ extensor surfaces, including the upper arms, thighs, cheeks, and buttocks.
The condition is also generally referred to as chicken skin because it causes patches of rough-feeling bumps on the skin.
These small patches of bumps are dead skin cells plugging hair follicles. It may sometimes appear brown or red.
Keratosis pilaris may first appear in childhood, like in some cases, and then progresses, becoming most extensive during puberty. Due to its prevalence, it is considered more of a ”skin type” instead of a medical condition to skin specialists.
With most affected individuals being adolescents, about 50% to 80% are affected. It has also been observed in the adult population, with 40% of the adult population affected.
Keratosis pilaris is known to worsen in the winter periods when the skin tends to dry out during pregnancy.
Even with these statistics, Keratosis pilaris seems to be an underreported skin condition and may be mistaken for similar conditions.
The prevalence of this skin condition may be higher; however, it affects any race and sex.
Classification
Generally, Keratosis pilaris is described in connection with other dry skin conditions such as ichthyosis, dry skin, vulgaris, atopic dermatitis, and including those of allergies and asthma. There are various types of Keratosis pilaris.
The several variations include:
- Keratosis pilaris rubra is characterized by red, inflamed bumps or papules which can form on the arms, head, and legs.
- Keratosis pilaris Alba forms rough, bumpy skin with no irritation.
- Keratosis pilaris rubra faceii appears as a reddish rash on the cheeks.
- Keratosis pilaris atrophicans faciei.
- Papular profuse precocious Keratosis pilaris.
- Eyrthromelanosis follicularis faciei et colli.
Keratosis pilaris is not known to hold any long-term health implications, and it is not associated with increased mortality or morbidity.
Unlike most speculations, the Keratosis pilaris is not associated with goosebumps that result from muscle contractions; the only similarity between goosebumps and keratosis pilaris is that both conditions occur in the area where the hair shat exist on the skin.
Causes
Keratin is a complex protein found in the skin that protects the skin from harmful substances and infection.
Keratosis pilaris is a skin condition resulting from keratin buildup (excess keratin); a buildup blocks the opening of hair follicles, resulting in rough, bumpy patches on the skin.
This condition, as earlier established, is prevalent, but the causes of keratin buildup or accumulation under a hair follicle remain a mystery.
According to 18th-century medical works of literature, the condition presents an autosomal dominant mode of inheritance. Genetically suspected by specialists, mutations in filaggrin have correlations with RAS signaling cascade and Keratosis pilaris.
Follicular abnormalities presented by Keratosis pilaris may result from mutations in the filaggrin gene.
Also, Keratosis pilaris is commonly associated with atopic dermatitis; this association with the mutation tendencies suggests that Keratosis pilaris results from a loss of normal epithelial barrier function.
The pathophysiology path for Keratosis pilaris is also not clear, but a widely proposed theory is that abnormal follicular keratinization causes an infundibular plug to form.
These plugs also cause the formation of inflammatory papules, a hallmark feature of Keratosis pilaris.
Finally, sinuously coiled hairs are found in the lesions or keratin plug and may play a part in the inflammation and keratinization of Keratosis pilaris.
Symptoms
This first observed symptom of Keratosis pilaris is its appearance. Visible skin bumps similar to goosebumps or a plucked chicken’s skin on the affected area of the skin; hence it’s alias chicken skin.
Bumps of Keratosis pilaris can appear anywhere hair follicles exist on the skin; that is why these bumps never occur on the feet’ palms or sole.
Common sites include the upper arms and thighs; in extension, the lower legs, forearms, or buttocks can be affected.
Some other Keratosis pilaris symptoms include:
- Itchy irritable skin
- Dry skin
- Redness around bumps
- Sandpaper-feeling bumps
- Bumps appear in various colors depending on skin tone; pink, red, brown, black, or flesh-colored.
Symptoms may worsen during puberty and pregnancy; it generally develops during childhood and improves over time.
A study was conducted in examining the course of Keratosis pilaris resolute 35% of patients with the condition improved over time, while 43% of patients had persistence in their condition. In 22% of patients, Keratosis pilaris worsened overtime.
The severity of Keratosis pilaris can also vary with the changing of seasons. During summer, 49% of patients noticed an improvement, while in winter months, 47% saw worsening of their condition.
This seasonal change was attributed to the reduced moisture content of the air during winter.
Risk factors of Keratosis pilaris
Anybody is likely to develop Keratosis pilaris, but it is most common in some set of people and often begins from the period of late infancy to adolescence.
Individuals at higher risk of developing Keratosis pilaris include:
- Women
- Obese people
- Dry skin
- Hay fever
- Eczema
- Ichthyosis
- Children during puberty
- Celtic ancestry
Keratosis pilaris typically clears up in a person’s mid-20s. In most cases, it is entirely gone by the age of 30. Hormonal changes during pregnancy can also influence the prevalence of Keratosis pilaris, especially in fair-skinned people.
Diagnosis of Keratosis pilaris
This skin condition is diagnosed clinically based on history and physical examination, as the doctor investigates the onset, location, appearance, and symptoms of the epidermal lesions.
The doctor looks out for numerous small inflammatory papules with a follicular association in the typical areas. Edema (dropsy) and erythema (abnormal redness) may accompany some lesion if the patient has interfered with the papules to extra keratotic material.
However, an evaluation of the affected skin lesions with a dermatoscopy may help in the diagnosis. During visualization with a dermatoscope, abnormalities of the hair follicle will be displayed.
Thin and short hair shafts can also be embedded within the stratum corneum. A biopsy may not be necessary for diagnosing Keratosis pilaris.
Differential Diagnosis of Keratosis pilaris
The differential diagnosis of Keratosis pilaris is some other skin conditions that can present similar symptoms as Keratosis pilaris.
These conditions may include:
Eratosis pilaris rubra
Eratosis pilaris rubra is a variant of Keratosis pilaris with more prominent erythema and widespread skin association without atrophy or hyper-pigmentation.
Ulerythema ophryogenes
Ulerythema ophryogenes is also a Keratosis pilaris variant, but it is uncommon. It affects young adults and is characterized by follicular papules on the cheeks and eyebrows, often accompanied by scarring, atrophy, and alopecia.
Lichen nitidus
Lichen nitidus is a skin condition that features flat-topped shiny pinpoint flesh-colored papules that are typically asymptomatic. The most common site of formation is on the trunk or flexural areas.
Ichthyosis Vulgaris
Ichthyosis Vulgaris involves symmetric and characteristic thick dark scaling and desquamation, particularly on the lower extremities and sparingly on the face.
Kyrle disease
This common skin condition is associated with diabetes and chronic renal failure (CRF). In this situation, large parafollicular papules with central keratin plugs are formed on the legs, and these papules are characterized by intense itching.
Darier disease
This is also known as Keratosis follicularis; it is an autosomal dominant genodermatosis known by its yellow-brown, malodorous, greasy, and hyperkeratotic papules in seborrheic regions of the body such as the chest, back, forehead, scalp, and nasolabial folds such as the groin, and axilla.
Acne
These are papules, pustules, and comedones present on sebaceous body areas, mostly in teenagers.
Eruptive vellus hair cysts
These are symmetrically distributed yellowish follicular papules containing small vellus hair. Eruptive vellus hair cysts may appear on the chest, flexor extremities, and face.
Trichostasis spinulosa
Trichostasis spinulosafeatures dark follicular papules, tiny bumps associated with 10-25 plugs of hair commonly found on the face, especially the nose, trunks, or arms.
Other conditions that dermatologists may mistaken for Keratosis pilaris include:
- Viral-associated trichodysplasia
- Keratosis spinulosa
- Keratosis follicularis spinulosa decalvans
- Follicular hyperkeratosis
Treatment of Keratosis pilaris
Many treatment and home health care options recipes are available for fighting Keratosis pilaris.
Most times, there are outstanding temporary improvements following routine skincare programs of lubrication with lotion. Generally, treatment needs to be continuous.
There is no universally effective treatment or available cure for Keratosis pilaris. Importantly, no one therapy is uniformly effective in all individuals, so Complete clearing may not be attainable.
A dermatologist (a physician specializing in skin and skin conditions) may recommend laser treatment or a moisturizing treatment for itchy, dry skin to improve skin appearance from a keratosis rash.
Over-the-counter prescription topical creams can also remove dead skin cells, and some may prevent hair follicles from being blocked, though it is advisable to confirm usage from a doctor.
Other treatment approaches generally suggested by a dermatologist include:
- Retinol creams
- Microdermabrasion, an intense exfoliating treatment
- Chemical peels
However, to avoid side effects caused by acids in topical creams, it is very needful to seek counsel from a dermatologist before applying a treatment.
Adverse side effects may appear as:
- Irritations
- Dryness
- Redness
- Stinging
Summary
Most people may be skeptical about the use of prescription topical cream or moisturizer containing lactic acid or glycolic acid to treat their Keratosis pilaris condition.
If this is the case, there are a few techniques that can be applied at home such as using natural salicylic acid.
Although Keratosis pilaris cannot be cured, these home cares can assist in minimizing small bumps, itching, and irritations:
- Taking short warm baths to help unclog and loosen spores. During these baths, rub the skin with a stiff brush to potentially remove bumps. It is imperative not to spend a long time as a long warm bath can remove the body’s natural oil.
- The use of daily exfoliate can improve the appearance of the skin. Dermatologists suggest the use of pumice stone to gently remove dead skin.
- Hydrating lotions containing alpha hydroxy acid (AHAs) like lactic acids can rehydrate dry skin and encourage cell turnover. Glycerin can also soften bumps, while rose-water can soothe skin inflammation; these can be purchased in beauty shops.
- Avoid tight clothing
- Make use of humidifiers. Humidifiers add moisture to the air in any room; this helps the skin maintain its moisture and prevents dryness and itchy flare-ups.
Sources;
- Keratosis pilaris classifications https://www.medicainenet.com/keratosis_pilaris/article.htm
- Living with Keratosis pilaris https://familydoctor.org/condtion/keratosis-pilaris/
- Treatment of Keratosis pilaris https://www.healthline.com/health/keratosis-pillaris#5-home-remedies
- Causes and Symptoms of Keratosis pilaris https://www.statpearls.com/ArticleLibrary/veiwarticle/23873
- Diagnosis and differential diagnosis of Keratosis pilaris https://www.dermatologyadvisor.com/home/decisio-support-in-medicine/dermatology/keratosis-pilaris-and-variants/