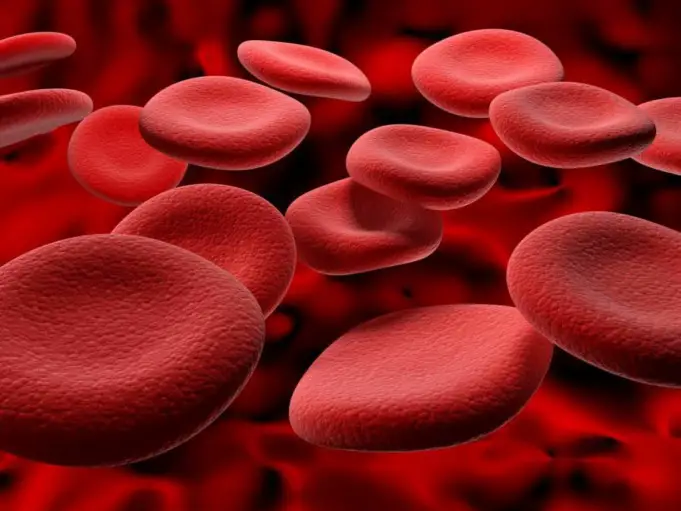
Hemoglobin, also known as Hb or Hgb, is the iron-containing protein molecule in the red blood cells (erythrocytes) in almost all vertebrates, which transports oxygen from the lungs or gills to the body tissues.
There, by aerobic respiration, the oxygen released provides power for the functioning of the organism in a process known as metabolism. Then hemoglobin returns carbon dioxide –a by-product of metabolism- from the tissues back to the lungs
Hemoglobin consists of four protein molecules that are connected. In adults, normal hemoglobin levels contain two alpha globulin chains and two beta-globulin chains.
Normal hemoglobin levels in fetuses and infants consist of two gamma chains two alpha and chains. As the child grows, beta chains gradually replace the gamma chains.
This forms a typical hemoglobin structure. There are 12 to 20 grams of hemoglobin in every 100 ml of blood in a healthy individual.
Each chain of globulin consists of an iron-containing porphyrin compound known as heme. Inside the heme compound exists an iron atom that is important in the transportation of oxygen and carbon dioxide in our blood.
The iron contained in the hemoglobin is also responsible or the bright red color of blood. This turns a dark red or brownish-red color on exposure to air due to oxidation.
Hemoglobin also plays a vital role in maintaining the shape of the red blood cells. Red blood cells are round with narrow centers that resemble a donut without a hole in the middle in their natural state.
Abnormal hemoglobin structure disrupts the shape of red blood cells and impedes their regular function and flow through the blood vessels. A given example is the sickle-shaped red blood cells, as seen in those with sickle cell anemia.
In the case of sickle cell anemia, Hemoglobin S is the variant of hemoglobin is present. It is a severe hereditary form of anemia in which the cell becomes crescent-shaped in the absence of oxygen.
These sickle-shaped cells die prematurely and block the tiny blood vessels, potentially causing an obstruction and leading to tissue damage.
This hereditary condition commonly found in people of African descent, although the disease also occurs in persons of Mediterranean, Indian, or Middle Eastern descent.
Hemoglobin can also be found outside red blood cells. Other cells that contain hemoglobin include macrophages, lungs, hepatocytes, A9 (dopaminergic neurons in the substantia nigra, mesangial cells in the kidney, and retinal pigment epithelium.
However, in these tissues, hemoglobin does not carry oxygen; instead, it functions and an oxidant and an iron metabolism regulator.
How is Hemoglobin measured?
Hemoglobin is measured during a routine complete blood test (CBT) of a blood sample. There are several methods of checking hemoglobin levels, and most are by machines designed to perform different blood tests.
Inside the machine, red blood cells are broken down to extract the hemoglobin into a solution. The extracted hemoglobin comes in contact with a chemical containing cyanide, which binds tightly with the hemoglobin molecule to form cyanomethemoglobin.
The amount of hemoglobin can be determined by how much light passed through it. The light is precisely at a wavelength of 540 nanometers.
Hemoglobin in the blood is expressed in grams per deciliter (g/dL). Low levels of hemoglobin in the blood indicates a low level of oxygen in the blood
Normal values of hemoglobin are dependent on a person’s age and sex. It may vary slightly between test systems and by what the doctor determines to be normal for their patients. Below are ranges for what is generally accepted as normal:
For infants
Birth: 13.5 to 24.0 g/dl
- Below 1 month: 10.0 to 20.0 g/dl
- Between 1-2 months: 10.0 to 18.0 g/dl
- Between 2-6 months: 9.5 to 14.0 g/dl
- Between 0.5 to 2 years: 10.5 to 13.5 g/dl
- Between 2 to 6 years: 11.5 to 13.5 g/dl
- Between 6-12 years: 11.5 to 15.5 g/dl
For females
- Between 12-18 years: 12.0 to 16.0 g/dl
- Above 18 years: 12.1 to 15.1 g/dl
For males
- Between 12-18 years: 13.0 to 16.0 g/dl
- Above 18 years: 13.6 to 17.7 g/dl
High levels of Hemoglobin
High hemoglobin levels could imply a rare blood disease known as polycythemia. It causes the body to produce too many red blood cells, making the blood to be thicker than usual.
This leads to heart attacks, clots, and stroke. It is a severe lifelong condition that can be fatal if not treated properly.
High levels of hemoglobin can also be caused by dehydration, living at high altitudes, and smoking. It has been associated with other conditions like lung and heart disease.
Low Levels of Hemoglobin
Low hemoglobin levels are indicative of anemia. There are different kinds of anemia, and they include:
- Iron-deficiency anemia: This is the most common type of anemia. It occurs when the person does not have sufficient iron in their body and cannot produce the hemoglobin it needs. Anemia is usually caused by blood loss as well as poor iron absorption.
- Vitamin-deficiency anemia: This occurs when there are low levels of vitamin B12 or folic acid in the diet. This type of anemia changes the shape of the erythrocytes (red blood cells) and reduces their efficiency.
- Pregnancy-related anemia: This is a kind of iron-deficiency anemia, which occurs because pregnancy and childbirth require a significant amount of iron.
- Sickle cell anemia: An inherited condition where the hemoglobin protein is an abnormal crescent shape. It means the erythrocytes are sickle-shaped and hard, which stops them from flowing through small blood vessels.
- Hemolytic anemia: This type of anemia occurs as a result of another existing condition. It can also be inherited. Hemolytic anemia occurs when the red blood cells are broken up in the bloodstream or the spleen.
- Aplastic anemia: This is a disorder in which the immune system attacks the stem cells that form blood in the bone. It results in fewer red blood cells.
Anemia is also caused by other conditions such as chemotherapy for the treatment of cancer, and kidney disease. The former affects the body’s ability to make red blood cells.
Infants have temporary anemia between 6-8 weeks old. It occurs when they run out of the red blood cells they are born with, but their bodies have not made new red blood cells. This condition does not affect the baby adversely unless they are sick for some other reason.
Babies can also have anemia from breaking down cells too quickly, which results in yellowing skin, a condition known as jaundice. It usually occurs if the mother and baby have incompatible blood types.