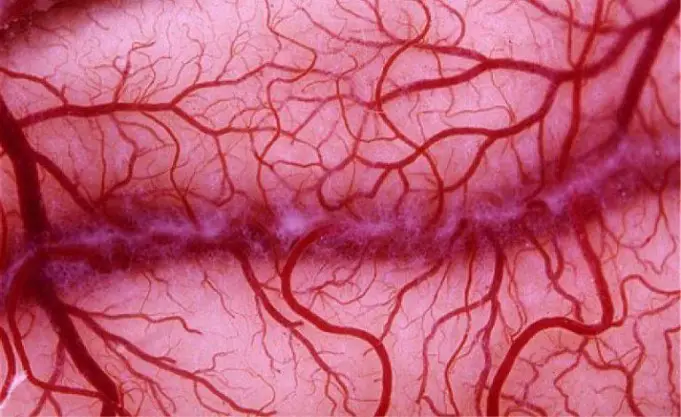
Coronary microvascular disease, also known as small artery disease or small vessel disease is a heart condition in which the walls and the inner lining of the coronary artery blood vessels are damaged. The damage to these tiny blood vessels can cause spasms and reduced blood flow to the heart.
The disease is characterized by symptoms that include shortness of breath, chest pain, and fatigue – symptoms that are similar and sometimes just as debilitating as those of coronary artery disease, which occurs due to buildup from cholesterol in the larger vessels of the heart. However, unlike heart disease, microvascular disease is challenging to diagnose.
Microvascular disease is more common in women and people who have diabetes, high blood pressure or a family history of cardiomyopathy. The condition can be fatal if left untreated.
Signs and Symptoms of Microvascular Disease
The symptoms of microvascular disease often mimic those of a heart attack. These symptoms include:
- Fatigue
- Shortness of breath
- Nausea
- Sweating
- Fainting
- Dizziness
- Chest pain and pressure, usually lasting longer than 10 minutes
- Pain in the mandible, neck, left shoulder, and arm, back, or abdomen
Seek medical attention immediately if you are experiencing chest pain and other symptoms like shortness of breath, nausea, dizziness, sweating or pain that radiates from your chest to your arms or neck.
Causes and Risk Factors of Microvascular Disease
The damage caused by microvascular diseases affects the ability of the small blood vessels to dilate, resulting in an inadequate flow of oxygen-rich blood to the heart.
The damage may be caused by:
- High blood pressure
- Obesity
- High cholesterol
- Diabetes mellitus
Microvascular disease will force your heart to work harder to pump blood to your body if left untreated. This pressure could trigger coronary artery spasms, a heart attack, heart failure, or even death.
Risk factors of microvascular disease include:
- High blood pressure
- Tobacco use
- Unhealthy cholesterol levels
- Unhealthy diet
- Obesity
- Sedentary lifestyle
- Estrogen deficiency, in women
- Insulin resistance
- Increasing age, men older than 45 and women older than 55
- Polycystic ovarian syndrome
- Chronic inflammation
Diagnosis
It can be challenging trying to diagnose microvascular disease. A medical professional would have to evaluate the patient’s symptoms, medical history, and family history.
The procedures used to diagnose microvascular disease are generally the same as those used in checking for other types of heart disease. These procedures show the function and structure of the larger coronary arteries and other parts of the heart. They may also indicate coronary artery blockages. The tests may include:
- Stress testing with nuclear imaging
- MRI
- CT scan or CT angiography scan
- Positron emission tomography (PET) scan
- Coronary angiogram, which is invasive and requires left heart catheterization
If there are no significant blockages in your larger coronary arteries, doctors carry out an invasive test which involves injecting different medications into a coronary artery, to check for blockages in your small arteries during a left heart catheterization.
This procedure is known as endothelial dysfunction test. This allows the doctor to measure the blood flow through your small vessels.
Treatment
Treating microvascular disease involves using medications to relieve pain and control the dilation of the small blood vessels that could cause a heart attack.
The doctor could prescribe:
- Beta-blockers: Drugs such as propranolol and bisoprolol (Zebeta), slow your heart rate and decrease your blood pressure.
- Nitroglycerin: Nitroglycerin tablets, sprays, and patches can help alleviate chest pain by relaxing your coronary arteries and improving blood flow.
- Statins: These medications help to lower cholesterol, which contributes to the narrowing of the arteries. They also help relax the blood vessels of the heart and treat blood vessel damage.
- Calcium channel blockers: These blockers help relax the muscles around the coronary arteries and cause the vessels to open, which increases blood flow to the heart. They also control high blood pressure.
- Angiotensin II receptor blockers (ARBs): They help relax your blood vessels, which lowers blood pressure and makes it easier for the heart to pump blood.
- Angiotensin-converting enzyme (ACE) inhibitors: Drugs such as benazepril and lisinopril help open the blood vessels and lower the blood pressure.
- Aspirin: Aspirin can reduce inflammation and prevent blood clots.
- Ranolazine (Ranexa): This drug eases pain in the chest by altering sodium and calcium levels.
You’ll need to see the doctor regularly for checkups if you are diagnosed with microvascular disease. The doctor will determine how often you’ll need to be examined, depending on the severity of your condition.
Sources
- Coronary Microvascular Disease (MVD) – heart.org
- Small Vessel Disease – Mayo Clinic
- What is Small Vessel Disease – Healthline
- Microvascular Dysfunction – Stanford Health Care