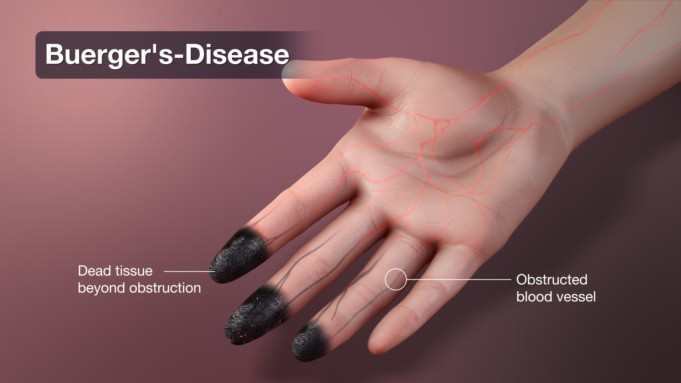
Buerger’s disease also referred to as thromboangitis obliterans (TAO), is a rare medical condition that affects the small blood vessels of the hands and legs.
The condition is thought to be a result of extensive tobacco use; the disease is characterized by inflammation and thrombosis of small and medium-sized arteries of the arms and feet with recurs and progresses in stages, beginning distally and proceeds proximally involving 5 to 10 cm lengths of blood vessels.
Buerger’s disease has a remarkably strong yet poorly understood association with cigarette smoking. The condition has not yet been discovered to occur in the absence of exposure to tobacco.
The disease features arterial obliteration which leads to the development of collateral vessels with a ‘corkscrew’ appearance on angiography.
Blood supply is cut-off the finger-tips and toes due to vessel swelling and formation of blood clots; this can cause severe pain, tissue damage, and even gangrene (decay of body tissues). In some cases, amputation may be required.
Buerger’s disease was first discovered in 1879 by a German physician called Felix Von Winiwater. It was later described in detail by Leo Buerger in 1908 in New York where he termed the condition presenile spontaneous gangrene after a study into the amputations in 11 patients.
Famous cases of the rare condition that gave it popularity in the 90’s was a case of King George VI (father of the Queen of England), who was diagnosed with Buerger’s disease on 12 November 1948. On 12 March 1949, the King underwent a successful lumbar sympathectomy, however, he didn’t quit smoking.
Study reveals that Buerger’s disease is most common in South Asians, Israel, Japan and India than in United States and Europe. Regions who often smoke cigarettes made of raw tobacco (bidis).
It has also been discovered to affect more males than females at a 3:1 ratio; though the global prevalence of the disease is still not clear, in the USA, it has decreased from 140 per 100,000 in 1947 to 8-12 per 100,000 as the prevalence of smoking has declined.
Classification on Buerger’s Diseas
Comparing cases of Buerger’s disease overtime has revealed the different types and sizes of the corkscrew collaterals.
Based on this, Buerger’s disease is classified presently into four (4) subtypes; these subdivisions of the condition also indicate the severity of disease, they include:
- Type 1: artery diameter greater than 2mm, helical sign
- Type II: diameter between 1.5mm and 2mm, medium helical sign
- Type III: diameter between 1mm and 1.5mm, this is the small helical sign type.
- Type IV: artery diameter less than 1mm, tiny helical sign.
Stages of Disease Development
Thromboangitis obliterans (TAO) or Buerger’s disease is a segmental vascular disease that causes occlusion and inflammation of the small-sized vessels.
Buerger’s disease vasculitis is quite unique as it features a hypercellularity with intraluminal thrombi (high rate of internal blood clotting) within the blood vessel wall that spares the elastic internal laminae of the vessel wall.
In the initial stage of development of the condition, otherwise known as the acute phase, the following occurs:
- The external lamina of the vessels of the distal extremities (fingertips and toes) are usually affect first by inflammatory thrombi (blood clots)
- The blood clots cause vessel occlusion (vessel blockage) while leukocytes (white blood cells) and giant cells infiltrates the vessel margins.
- Superficial veins in particular may show evidence of thrombophlebitis (inflammation of the veins), and this is characteristic and diagnostic of the acute phase.
The intermediate or subacute phase is known by the progressive accumulation of thrombi within the vessel.
The last phase which is known as the chronic phase features a continuation of thrombi accumulation with fibrosis, ending with the resolution of inflammation.
In the chronic phase:
- The disease vessels are not distinct from other vascular disease.
- Obliteration of the supplying vessels of the extremities suffers severe ischemia and this may lead to gangrene and superimposed infection, mostly of the fingers and toes.
Causes of Buerger’s Disease
Buerger’s disease mostly affects the tibial, popliteral and radial arteries and the development of the disease may be the result of an immunologic phenomenon that leads to vascular dysfunction and development of inflammatory thrombi.
Persons with Buerger’s disease have been pointed out to have hypersensitivity against tobacco extracts that are injected intradermally.
Pathophysiological research on the condition have unveiled evidence that demonstrates that there is an increased cellular response against collagen type I and III with increased levels of circulating anti-endothelial cell antibody upon exposure to tobacco and tobacco extracts; via smoking and other invasive forms of consuming tobacco (smoking tobacco is critical to the initiation, progression and recurrence of Buerger’s disease).
This increased cellular sensitivity leads to an impaired relaxation mechanism of the peripheral vessels. Cytokines are also thought to be produced in large amounts and may lead to the activation of inflammatory signals.
Also, the presence of elevated anti-cardiolipin antibodies is thought to be indicative of prognosis and severity. Rickettsial infection has been proposed to be one of the causes of Buerger’s disease.
The autoimmune phenomenon that serves as an underlying genetic cause of Buerger’s disease is linked genes that have been identified to be associated with tobacco hypersensitivity in patients, these genes include DRBI*0405, DQAI*03, DQBI*0401, DPBI*0501, HLA-A54, HLA-A9, and HLA-B54.
On gross pathology, ischemia, cyanosis, rubor, ulceration, and dry or wet gangrene with or without autoamputation are the characteristic findings of Buerger’s disease.
Risk factors of Buerger’s Diseas
The population who are more at risk in developing Buerger’s disease is tobacco smokers. Other potent risk factors include:
- Male sex
- Age between 20 to 45 years
- Those with Rickettsial infection
- South Asian or Middle Eastern descent
- Those with medical history of Raynaud’s disease or autoimmune disease
Symptoms of Buerger’s Diseas
Symptoms are most likely to affect two or more limbs and they may include:
- Fingers or toes that appear pale, red, or bluish (cyanosis) and feel cold to touch.
- Sudden severe pain in the hands and feet; burning sensations or tingling.
- Pain in the hands and feet most often occurs when resting.
- Pain in the legs, ankles, or feet when walking (intermittent claudication). The pain is often located in the arch of the foot.
- Skin changes or small painful ulcers on the fingers or toes
- Occasionally, arthritis in the wrist, ankle or knees develops before the blood vessels become blocked.
Diagnosis of Buerger’s Disease
No single test can check for Buerger’s disease. Doctors and other clinicians try to diagnose the condition by checking the individual’s use of tobacco and physically examine the symptoms.
Laboratory tests to check for blood flow in order to rule out other diseases that cause similar symptoms.
Other tests that can be used to diagnose for Buerger’s disease include:
The Allen Test
This test is a blow flow test. First, the doctor asks the patient to squeeze his/her hand into a hard fist, which pushes blood out of the hand and the doctor presses on the arteries of the wrist to slow the flow of blood back into your hand.
At this point, the hand will lose color. When the patient opens his hand, the doctor releases the pressure over the artery on one side of the wrist and then the other side.
If it takes a while for the hand to return to its usual color, it may be a sign of Buerger’s disease.
Angiogram
This is an X-ray that checks for blocked blood vessels in the arms and legs. A thin tube called a catheter, is inserted into the artery and harmless dye is pumped into the artery and quickly, an X-ray is conducted to look at the blood vessels.
Similar pictures can be produced by a CT or MRI scan.
Differential Diagnosis
Other medical conditions can cause similar symptoms as Buerger’s disease, such as ischemic vasculitis. Buerger’s disease must be differentiated from other diseases, such as raynaud phenomenon, thromboembolic disease, atherosclerosis, repeated trauma, vasculitides, frostbite, scleroderma and systemic lupus erythematosus.
Complications
When left untreated, 75% of persons with Buerger’s disease may suffer a relapsiong and remitting course, while 20% may progress and 5% may have a benign course of Buerger’s disease. Common complications of Buerger’s disease include:
- Amputation
- Gangrene
- Loss of circulation beyond affected digits.
Amputation is common and more severe in patients who continue to use tobacco, which often leads to vascular insufficiency. Buerger’s disease is rarely immediately fatal but a rather progressive life shortening disease.
Treatment of Buerger’s Disease
Actually, there is no treatment for Buerger’s disease. In order to prevent progression and control symptoms, tobacco consumption cessation is crucial; though cessation of tobacco consumption (smoking) does not reverse the damage already caused but limits the effect of Buerger’s disease.
Pharmacologic medical therapies for Buerger’s disease include palliative treatments, prostaglandin analogs, phosphodiesterase inhibitors, smoking cessation, calcium channel blockers, endothelin receptor antagonists and compression therapy.
Patients should be aware that these treatments approach are purely palliatives and do not reverse previous damage caused.
A prostaglandin analog such as Iloprost is especially effective in the intravenous form at reducing pain symptoms, better than low dose aspirin or lumbar sympathectomy.
Iloprost can facilitate smoking cessation and may be used to manage resting pain symptoms in those patients with critical limb ischemia.
Calcium blockers are used for patients whose main complaint is the Raynaud phenomenon. Those that prevent vasospasm (a condition leading to vasoconstriction) include the dihydropyridines such as nifedipine, nicardipine, and amlodipine.
Intermittent pneumatic compression (IPC) is used for patients whose main complaint is that of poor blood circulation in the extremities.
This therapy is able to increase the flow of blood through the arteries by decreasing the peripheral arterial resistance.
Other experimental therapies (therapies still in the trail stage) that can be used against Buerger’s disease include:
- Therapeutic angiogenesis: Patients with ischemic pain or non-healing ulcers may benefit from the use of angiogenesis that uses growth factors, such as intramuscular vascular endothelial growth factor, in order to promote the generation of blood vessels. Therapeutic angiogenesis has also demonstrated that it may reduce the occurrence of nocturnal resting pain.
- Autologous bone marrow mononuclear cell implantation: When the traditional revascularization treatment approach fails in those with severe peripheral artery disease, autologous bone marrow mononuclear cell implantation may be performed. The implantation may be able to relieve ischemic pain symptoms and decrease ulcer size.
- Analgesia: Non-steroidal anti-inflammatory drugs may be used to relieve pain symptoms, including naproxen, ibuprofen, indomethacin, diclofenac, and ketofen. Also, acetaminophen administered alone or with codeine or hydrocodone is very effective.
- Immunoabsorption therapy (bosentan and cilostazol): Immunoabsorption therapy and bosentan (endothelin receptor antagonist) have clinically demonstrated that they are effective in improving pain intensity and ulcer healing. Cilostazol (phosphodiesterase inhibitor) is a suppressor able to cause reactive hyperemia and therefore improve blood flow.
Prevention of Buerger’s Disease
The most effective measure for the prevention of Buerger’s disease is smoking cessation; this should include complete abstinence without the use of nicotine-containing anti-smoking aids, such as transdermal patches and gum.
However, the use of bupropion and varenicline for preventing cravings can be allowed.
Also, other effective ways to prevent Buerger’s disease and its complications entails debridement and dressing of the ulcers, avoiding exposure of the extremities to cold temperatures, surfaces, wearing protective footwear to avoid injury.
Lack of healing thereafter, early detection, and treatment of injuries in the extremities including the use of prophylactic antibiotics and vasoconstricting medications must be avoided.
Sources;
- Buerger’s Disease; http://www.cdc.gov/tobacco/campaign/tips/diseases/buergers-disease.html
- Buerger’s Disease; http://www.healthline.com/health/thromboangiitis-obliterans#outlook
- Buerger’s Disease; https://www.mayoclinic.org/diseases-conditions/buergers-disease/symptoms-causes/syc-20350658
- Buerger’s Disease; https://rarediseases.org/rare-diseases/buergers-disease/