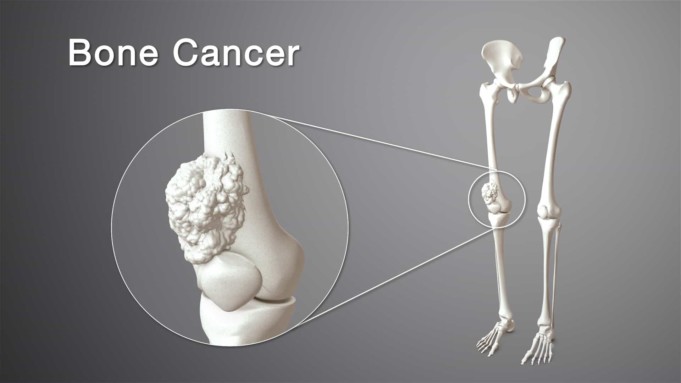
In any bone in any part of the body, bone cancer can begin, but it most commonly affects the pelvis or long bones in the arms and legs.
Bone cancer is unusual and makes up less than 1% of all cancers. Noncancerous bone tumours are generally much more common than cancerous tumours.
Cancers that begin somewhere else in the body and spread to the bone (metastasize) are not referred to as “bone cancer” Instead, certain cancers, including breast cancer that has metastasized to the bone, are named for where they started.
Some bone cancer forms occur mainly in children, while others often affect adults. The most common procedure is surgical removal, but chemotherapy and radiation therapy can also be used.
Based on the type of bone cancer, the decision to use surgery, chemotherapy or radiation therapy can be determined.
Symptoms
Signs and symptoms of bone cancer include;
- Swelling near the affected region and tenderness
- Weakened bone that results in fracture
- Tiredness
- Bone pain
- An unintended loss of weight
When to see a doctor
Make an appointment with a doctor if you or your child experiences bone pain that;
- Comes and goes
- Worsening at night
- Over-the-counter pain relievers do not improve.
Causes
The cause is unclear for the majority of bone cancers. Hereditary factors have been related to a small number of bone cancers, while some are linked to past exposure to radiation.
Types of bone cancer
Bone cancers, depending on the type of cell where cancer started, are broken down into different forms.
Among the most common forms of bone cancer are;
- Osteosarcoma. The most prevalent type of bone cancer is osteosarcoma. The cancerous cells generate bone in this tumour. Most commonly, this variety of bone cancer occurs in children and young adults, in the leg or arm bones. Osteosarcomas may occur outside of the bones in unusual circumstances (extraskeletal osteosarcomas).
- Chondrosarcoma. The second most common type of bone cancer is Chondrosarcoma. The cancerous cells create cartilage in this tumour. In middle-aged and older adults, Chondrosarcoma commonly occurs in the pelvis, legs or arms.
- Ewing sarcoma. Ewing sarcoma tumours most often occur in children and young adults in the pelvis, legs or arms.
Risk factors
It’s not clear the exact causes of bone cancer, but doctors have discovered certain factors are associated with an increased risk, including;
- Inherited genetic syndromes. The risk of bone cancer includes Li-Fraumeni syndrome and hereditary retinoblastoma, is increased by some unusual genetic syndromes inherited by families.
- Paget’s disease of bone. Paget’s bone disease, which occurs most often in older adults, may raise the risk of later development of bone cancer.
- Radiation therapy for cancer. Exposure to high doses of radiation, such as those delivered during cancer radiation therapy, raises the risk of potential bone cancer.
Diagnosis
The location and size of bone tumours, and whether the tumours have spread to other areas of the body, can be determined by imaging tests. Recommended types of imaging tests depend on the specific signs and symptoms.
Tests can involve;
- Bone scan
- Computerized tomography (CT)
- Magnetic resonance imaging (MRI)
- Positron emission tomography (PET)
- X-ray
Needle or surgical biopsies
For laboratory research, your doctor may prescribe a procedure to extract a sample of tissue (biopsy) from the tumour. Testing will tell your doctor if there is cancer in the tissue and if so, what kind of cancer you have.
It can also reveal whether tumour cells are rapidly or slowly developing.
Types of biopsy methods used to diagnose cancer of the bone include:
- Inserting a needle through the skin and into a tumour. Your doctor sticks a thin needle into the skin during a needle biopsy and directs it through the tumour. Your doctor uses the needle to extract tiny bits of tissue from the tumour.
- Surgery to extract a tissue sample for testing. Your doctor makes an incision through the skin during a surgical biopsy and removes either the whole tumour or a part of it.
Determining the kind of biopsy the patient needs and the details of how it should be done to allow the medical team to prepare carefully.
Doctors need to conduct the biopsy in a way that would not interfere with potential bone cancer removal surgery. For this reason, prior to your biopsy, ask your doctor to refer you to a team of doctors with extensive expertise in the treatment of bone tumours.
Stages of bone cancer
When your doctor confirms a bone cancer diagnosis, he or she attempts to assess the degree (stage) of cancer because it will direct the choices for treatment.
Factors to be taken into account include;
- The tumour’s size
- How fast does cancer grow?
- The number of impacted bones, such as the spine’s adjacent vertebrae
- If the bone cancer has spread to other body parts
Roman numerals, ranging from 0 to IV, signify the phases of bone cancer. The lowest stages show a smaller and less aggressive tumour. Stage IV is when the bone cancer has spread to other parts of the body).
Treatment
Your bone cancer care choices are dependent on the type of cancer that you have, the stage of the bone cancer, your general health and your preferences.
Different cancers of the bone respond to different therapies, and your doctors will help direct you to the right treatments for your cancer.
Some bone cancers, for example, are treated by surgery alone; some by surgery and chemotherapy; and some by surgery, chemotherapy and radiation therapy.
Surgery
The goal of the surgery is to remove the cancerous tumour as a whole. In most cases, this requires special procedures, along with a small amount of healthy tissue that surrounds it to extract the tumour in one single piece.
The surgeon will replace the missing bone with some bone from another part of your body, with bone bank material, or with metal and hard plastic substitute.
Bone cancers that are very large or situated on the bone at a difficult point can need surgery to remove all or part of the limb (amputation). Amputation is becoming less common as other therapies have been developed.
If amputation is required, you will probably be equipped with an artificial limb and will learn to do daily tasks using your new limb through training.
Chemotherapy
In order to destroy cancer cells, chemotherapy makes use of powerful anti-cancer medications, usually administered via a vein (intravenously).
This method of treatment, however, works better for some types of cancer of the bone than for others. Chemotherapy, for example, is usually not very good for Chondrosarcoma but is an essential component of osteosarcoma and Ewing sarcoma treatment.
Radiation therapy
To destroy cancer cells, radiation therapy uses high-powered energy beams, such as X-rays. You lie on a table during radiation therapy, while a special machine travels around you and focuses the energy beams at accurate points on your body.
Before an operation, radiation therapy is also used because it can compress the tumour and make it easier to remove. In turn, this will help decrease the possibility that amputation would be required.
In people with bone cancer that can not be eliminated by surgery, radiation therapy can also be used. Radiation therapy may be used following surgery to destroy any cancer cells that may be left behind. Radiation therapy could help monitor signs and symptoms, such as pain, for people with advanced bone cancer.
Coping and support
A cancer diagnosis can be frustrating. With time one will find ways to cope with the uncertainty, distress and fear of cancer. Until then, you might find the following tips useful:
- Learn enough about bone cancer to make decisions about your care. Ask your doctor about your bone cancer, and also ask about your options for treatment and your prognosis, if you wish. You might become more secure in making treatment decisions as you learn more about bone cancer.
- Keep friends and family close. It will help you deal with bone cancer by keeping your close relationships strong. The logistical support you would need can be provided by friends and family, such as helping to take care of your house while you’re in the hospital. And when you feel overwhelmed by cancer, they can serve as emotional support.
- Find someone to talk with. Find a good listener who is able to hear you speak about your worries and hopes. This could be a member of a friend or family. Often beneficial can be the concern and knowledge of a counsellor, medical social worker, church member or cancer support group. Ask your doctor about your area’s support groups. Or search your phone book, library, or a cancer association, such as the American Cancer Society or the National Cancer Institute.
Preparing for your appointment
Start by making an appointment with your family doctor if you have any signs and symptoms that concern you. You may be referred to a specialist if your doctor believes that you might have bone cancer.
A team of specialists also treat bone cancer, which may include;
- Orthopaedic surgeons who specialize in operating on cancers that affect the bones (orthopaedic oncologists)
- Doctors who specialize in treating cancer with chemotherapy or other systemic medications (oncologists)
- Doctors who use radiation to treat cancer (radiation oncologists)
- Doctors who analyze tissue to diagnose the exact type of cancer (pathologists)
- Rehabilitation specialists who after surgery can help you recover
How to prepare
Since appointments can be short, and since there’s always a lot of ground to cover, being well-prepared is a good idea. Try the following:
- Be aware of any pre-appointment restrictions. Be sure to inquire at the time you make the appointment if there’s something you need to do in advance, such as limiting your diet.
- Write down any symptoms you’re experiencing, including those that might seem to be irrelevant to the reason you planned the appointment for.
- Write down key personal information, And any substantial pressures or recent changes in life.
- Make a list of all medications, vitamins or supplements which you take.
- Consider taking a friend or family member along. It can often be hard to recall all the specifics given during an appointment. Somebody who accompanies you can recall something you forgot or overlooked.
- Bring your previous scans or X-rays (both the images and the reports) along with other medical reports that are applicable to the appointment in this case.
Questions to ask
You will help make the most of your time together by planning a list of questions for your doctor. List your questions in case time runs out from most important to least important. Some specific questions to ask your doctor about bone cancer include:
- What sort of bone cancer am I suffering from?
- What is the stage of my bone cancer?
- What’s the extent of my bone cancer?
- Am I going to need some extra tests?
- What are my bone cancer care options?
- What are the chances that my bone cancer will be healed by treatment?
- What are the side effects of each treatment choice and the risks?
- Is therapy going to make it impossible for me to have kids?
- I have another health problem. How will bone cancer treatments affect my other conditions?
- Do you think there’s one therapy that is best for me?
- In my case, what would you suggest to a friend or family member?
- Can I see a professional? What is this going to cost, and is my insurance going to cover it?
- Can you suggest a doctor if I would like a second opinion?
- Are there any brochures that I can carry with me or other printed materials? What websites are suggested by you?
Don’t hesitate to ask any questions during your visit, in addition to the questions that you’ve planned to ask your doctor.
What to expect from your doctor
There are a variety of questions the doctor is likely to ask you. It can give more time to cover other points you want to discuss by being ready to answer them. Your physician may ask:
- When did you start feeling symptoms for the first time?
- Were your symptoms persistent or occasional?
- How seriously do your symptoms look?
- What appears to help the symptoms, if anything?
- What seems if anything to make the symptoms worse?
References:
- What are the Symptoms and Signs of Bone Cancer? CTCA
- Bone cancer Disease Reference Guide; Drugs.com
- Bone cancer – Diagnosis and treatment; Mayo Clinic