Atopic eczema or baby eczema can be a great cause of concern for parents, and most time, the home remedies that are available may not be as effective as we want them to be. In this article, we will discuss all there is to know about atopic eczema, including the possible causes and solution.
Studies show that about 13 per cent of children younger than the age of 18 in the United States of America have eczema, and that including atopic dermatitis or atopic eczema (which happens to be the most common type of eczema), according to a report that was published in the May–June of 2014 in the journal dermatitis.
This baby eczema, also known as infantile eczema, often persists through a person’s childhood and adolescence, and may even last into adulthood.
What is the cause of baby eczema or eczema in children?
Though a lot of studies have been carried out, researchers are yet to find out exactly what leads to eczema in babies. However, they believe that there is a chance of baby eczema being a result of a combination of environmental and genetic factors. Baby eczema or any other type of eczema is not contagious.
Infants stand a higher chance of developing eczema is their family members have a history of hay fever, asthma, or even eczema. While these conditions are not known to cause one another in any way, infants are more likely to develop asthma or hay fever if they have baby eczema.
Scientists are led to believe that eczema may be a result of an immune-system dysfunction that affects the human skin barrier and its ability to lock in moisture.
Eczema is not a single condition, but a general term that is used to describe several inflammatory skin conditions. Apart from atopic dermatitis, there are other types of eczema that commonly affect babies and young children including dyshidrotic eczema (foot-and-hand eczema), contact dermatitis, and seborrheic dermatitis, or scalp eczema (also known as cradle cap in babies)
The Environment and Baby Eczema Risk Factors
While baby eczema is an outcome of immune-system dysfunction, most likely from a genetic predisposition, researchers have found a number of possible risk factors.
For example, a study that was published in February 2018 suggested that kids have a higher risk of developing atopic eczema if their mums experienced situations of high-stress situations during pregnancy.
In a UK research that was published in the Journal of Allergy and Clinical Immunology in May 2018, the sociodemographic characteristics of around 675,000 children were analyzed in a primary-care database.
They discovered that the babies were more likely to be diagnosed with eczema if they fell into one of the following categories:
- Male
- Chinese
- Black Caribbean
- Bangladeshi
- Of high socioeconomic status
Baby Eczema and the Cradle Cap Symptoms
Baby eczema has been known to cause symptoms such as red rashes that could make the skin itchy, dry, and scaly. The red rash can also develop small bumps, which may smell or weep fluid. Other common symptoms may include:
- Redness and swelling
- Thickened skin
- Darkened skin around the eyes and on the eyelids
- Changes to the skin around the eyes, ears, and mouth
Cradle cap often causes symptoms that are not commonly seen in other kinds of infantile eczema, like a greasy yellow scale on the scalp that may appear in a thick layer covering the whole top part of a child’s head. Over time, the scales become flaky and rub off.
Most infants do not appear to be bothered by the cradle cap skin condition even though it sometimes itches.
A baby that has atopic dermatitis has a higher risk of other atopic (allergic) conditions, such as hay fever, asthma, and food allergies.
Progression of baby eczema
Baby eczema is often most prominent on the forehead, cheeks, and scalp of a baby within the first few months of their life, and it often tends to make the child’s skin look more weepy and red than at other ages.
Eczema can show up on other parts of the child’s body as well, including around the diaper area.
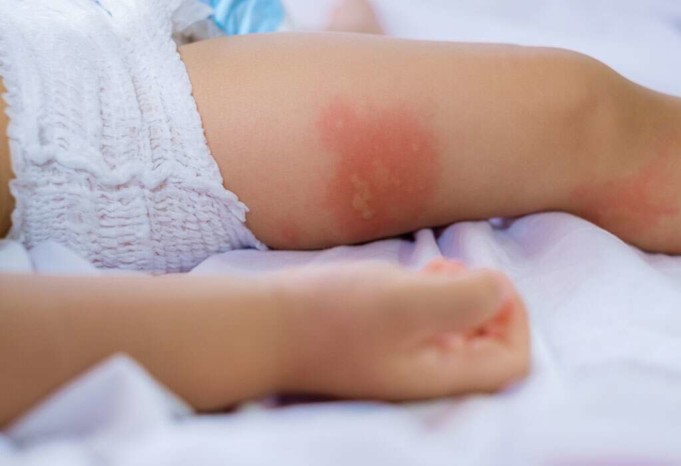
When the baby begins to crawl, which is usually between 6 months and 1 year, eczema will often affect the knees and elbows, which are the areas that rub on the ground. Also, the eczema rash may become infected, leading to a yellowish crust or little bumps of pus.
When the baby grows to age 2, eczema may start to appear on the inside of his or her elbows and behind the knees, as well as on the ankles, wrists, and hands. It may also show up around the eyelids and mouth.
This eczema tends to be scalier, thicker, and drier.
What Are the things that trigger the symptoms of Eczema?
Eczema usually is not a persistent condition, but a condition that is marked by long asymptomatic periods followed by flare-ups.
There are various environmental factors that may cause a person’s immune system to respond as if there is a harmful substance in the body, resulting in inflammation and worse symptoms of eczema.
These triggers may include a wide range of irritants and allergens, such as:
- Pet dander, dust mites, pollen, and mould
- Allergenic foods (such as soy, peanuts, and eggs)
- Clothing made of synthetic fibres or wool
- Scented products, like perfume, laundry detergents, and air fresheners, especially those that contain alcohol
- Cigarette smoke
- Excessive heat or dryness
- Skin infections
- Dry winter air with little moisture
- Stress
- Sweating
- Also, drool can irritate a baby’s cheeks, chin, and neck
Treatment for Baby Eczema
There is no known cure for atopic eczema, but the condition often becomes less severe over the years.
Treatment for baby eczema mainly focuses on dealing with skin dryness to prevent flare-ups and also to reduce skin inflammation. Doctors often recommend the strategies below to parents whose infants have eczema:
- Avoid giving your infant long hot baths (opt for cool or lukewarm water instead) and resist the urge to rub your baby’s skin too much, mostly with rough washcloths, towel or loofahs.
- Moisturize your child’s skin often with fragrance- and dye-free creams, ointments, and lotions, especially right after they get a bath.
- Dress your child in soft, breathable cotton clothing.
- Avoid the use of scented products.
- Keep your infant’s fingernails short to prevent scratches, which may damage the skin and further lead to infection and inflammation.
- Eliminate irritants and known allergens from your home as much as you can.
- Keep your infant cool to avoid constant sweating, possibly by making use cool compresses (a cool or wet washcloth), especially on the areas.
Consider making use of mittens on your infant’s hands if you must leave the child on its own for a short period of time, like when you are using the bathroom. This will go a long way to help prevent the child from scratching its skin when you are not around.
Your doctor may also recommend that you use other kinds of eczema treatments for your child, such as:
- Antihistamines
- Topical corticosteroids
- Antibiotic, antifungal, or antiviral drugs for skin infections
- Oral medications that help to suppress the immune system
- Topical calcineurin inhibitor
These are a few of the medications that your doctor may prescribe, but it also helps to make sure that your environment is neat, and you keep your baby cool in the heat.